Hormone imbalances affect millions of people, yet most patients receive generic treatment plans that ignore their unique biology. At NuMed DPC, we believe personalized treatment for hormone imbalance is the only approach that truly works.
Your hormones control everything from energy and mood to metabolism and sleep. When they’re out of balance, standard protocols often miss the root cause, leaving you frustrated and still struggling.
What Does Hormone Imbalance Actually Feel Like
Hormonal dysfunction rarely announces itself with a single, obvious symptom. Instead, it shows up as fatigue that coffee cannot fix, mood swings that feel disconnected from your circumstances, or weight gain that resists your usual diet and exercise efforts. Women commonly report hot flashes and night sweats, especially during perimenopause and menopause, alongside sleep disturbances that leave them exhausted despite spending eight hours in bed. Men experience low energy, reduced libido, brain fog, and mood changes that they often attribute to stress or aging rather than hormonal shifts. Some people notice their skin becoming oily or breaking out in acne, while others experience decreased libido, vaginal dryness, or changes in muscle mass and strength. The problem is that these symptoms overlap with dozens of other conditions-thyroid dysfunction, depression, sleep apnea, nutritional deficiencies-which means most patients bounce between providers, receiving treatments that address the surface complaint rather than the underlying hormonal dysfunction.
Why Generic Protocols Miss What’s Actually Wrong
Standard medical approaches treat symptoms in isolation. A patient reporting fatigue receives stimulants. Another with mood swings gets antidepressants. A third with weight gain hears the same advice: eat less and move more, despite the fact that a hormonal imbalance suppresses metabolism and increases hunger signals in ways that willpower alone cannot override. This fragmented approach ignores the reality that your hormones form an interconnected system-estrogen, progesterone, testosterone, cortisol, thyroid hormones, and insulin all influence each other. When one falls out of balance, it triggers a cascade of effects that generic protocols cannot address. Additionally, lifestyle factors like sleep duration, stress levels, gut health, and exercise patterns directly influence hormone production and metabolism, but standard care rarely examines these drivers.
The Hidden Costs of Treating Symptoms Instead of Causes
When a hormonal imbalance goes undiagnosed, the consequences extend far beyond discomfort. Women with untreated estrogen decline face increased osteoporosis risk after menopause, with bone density changes that can lead to fractures from minor falls. Heart disease remains the leading cause of death among women, and hormonal changes significantly influence cardiovascular risk, yet most patients never receive screening or preventive guidance tied to their hormonal status. Untreated testosterone deficiency in men accelerates muscle loss, weakens bones, and increases metabolic dysfunction. The condition affects roughly ten percent of women of reproductive age and requires ongoing management, yet many patients receive only fertility-focused care or insulin management without addressing the underlying hormonal drivers. The mental health impact proves equally serious. Hormonal fluctuations directly influence mood regulation, and conditions like PCOS and thyroid disorders trigger anxiety and depression. Patients end up on multiple medications addressing depression, anxiety, and sleep problems when the root cause, hormone imbalance, remains untreated.
Why Personalized Testing Changes Everything
The gap between standard care and effective treatment starts with diagnosis. Generic blood work often misses hormonal imbalance because it relies on population-wide reference ranges that ignore individual variation. A woman’s estrogen level might fall within the “normal” range yet still cause significant symptoms based on her unique physiology and life stage. Men’s testosterone levels fluctuate throughout the day, and a single test taken at the wrong time produces misleading results. Comprehensive hormone testing examines multiple markers-not just total hormone levels but also free hormone levels, binding proteins, and metabolic indicators-to reveal the actual picture of your hormonal status. This detailed assessment identifies whether your symptoms stem from insufficient hormone production, impaired hormone metabolism, excessive stress hormone output, or a combination of factors. Once testing reveals the specific imbalance, treatment can target the actual problem rather than guessing at a one-size-fits-all solution. Understanding your individual hormone profile also reveals which lifestyle modifications will have the greatest impact on your specific situation, allowing you to invest your effort where it matters most.
Moving From Diagnosis to Personalized Solutions
Identifying hormone imbalance represents only the first step. The real transformation happens when testing results guide a treatment plan built specifically for your body, your symptoms, and your goals. This is where personalized medicine diverges sharply from standard protocols-instead of applying the same approach to every patient, treatment adjusts to match your individual needs.
Root Cause Analysis in Hormone Treatment
What Tests Actually Reveal About Your Hormones
Comprehensive hormone testing differs fundamentally from the standard blood work most patients receive. Standard protocols check total hormone levels against population-wide reference ranges, which means a woman’s estrogen can fall within the normal zone while still causing severe symptoms, or a man’s testosterone can appear adequate despite producing obvious dysfunction. Effective diagnosis requires testing that examines free hormone levels, binding proteins, metabolic markers, and hormonal interactions rather than isolated numbers.

Free testosterone represents the hormone actually available to your cells, yet many clinics measure only total testosterone, missing the real picture. Testing should also include cortisol dysregulation assessment since cortisol patterns suppress other hormones and drive fatigue, anxiety, and weight gain. Morning serum cortisol has been proposed as an initial diagnostic tool, though comprehensive cortisol assessment reveals whether your rhythm is broken.
Thyroid assessment demands multiple markers: TSH alone misses central hypothyroidism and thyroid antibody problems that cause symptoms despite normal TSH. Insulin and glucose levels reveal metabolic dysfunction that drives weight gain and mood instability. The International Menopause Society White Paper from 2024 emphasizes that hormone therapy decisions depend on individualized assessment of symptoms and lab values rather than age-based protocols, underscoring why precise testing matters before any treatment begins.
Lifestyle Factors That Silently Drive Imbalance
Your daily choices shape hormone production more powerfully than most people realize. Sleep deprivation reduces testosterone by up to 15 percent the next day, according to sleep research, yet patients often receive hormone prescriptions while ignoring their five-hour sleep schedule. Excess belly fat actively produces estrogen through aromatase enzyme activity, which perpetuates an imbalance in both men and women.
Chronic stress elevates cortisol, which suppresses thyroid function and testosterone while increasing appetite and fat storage around the abdomen. Gut dysfunction impairs hormone metabolism because your liver and gut bacteria recycle estrogen and other hormones; poor digestive health or dysbiosis directly undermines hormone balance regardless of treatment. Nutrient deficiencies in vitamin D, zinc, and B vitamins limit your body’s ability to produce and metabolize hormones effectively.
High-intensity exercise without adequate recovery increases cortisol rather than optimizing it. These factors must be identified during assessment because no hormone therapy succeeds long-term if the lifestyle drivers remain unchanged. A personalized medicine approach examines your sleep patterns, stress levels, exercise habits, nutritional status, and digestive function alongside your labs to build a complete picture of what’s actually causing your symptoms.
Personalized Medicine Targets Root Causes, Not Symptoms
Once testing and lifestyle assessment reveal your specific imbalances and drivers, treatment becomes precise rather than generic. A woman with low progesterone and high cortisol needs a different intervention than a woman with normal progesterone but impaired estrogen metabolism. A man with low testosterone from poor sleep and excess weight requires a different strategy than one with primary testicular failure.
This distinction matters because treating the wrong problem wastes time and money while leaving you struggling. Functional medicine explicitly examines nutrition, sleep, stress management, gut health, and exercise patterns as part of hormone optimization rather than treating them as separate concerns. Health coaching helps you implement sustainable changes rather than expecting willpower to override hormonal signals.
Regular monitoring through follow-up labs and symptom tracking allows your provider to adjust treatment as your body responds, catching issues like elevated blood pressure or metabolic changes early. The personalized approach also respects your preferences and life circumstances; some patients prefer transdermal hormone delivery to avoid liver metabolism, while others need oral options that fit their routine. Treatment plans adjust based on your individual tolerance and response rather than following a standardized protocol.
This level of individualization requires accessible healthcare that provides longer appointments, easy lab access, and ongoing communication with your provider. The rushed fifteen-minute office visits that characterize standard care cannot support the detailed assessment and continuous adjustment that hormone balance demands. Your provider must have time to understand your complete health picture and modify your plan as circumstances change, which sets the stage for exploring the specific treatment strategies that work best for your unique situation.
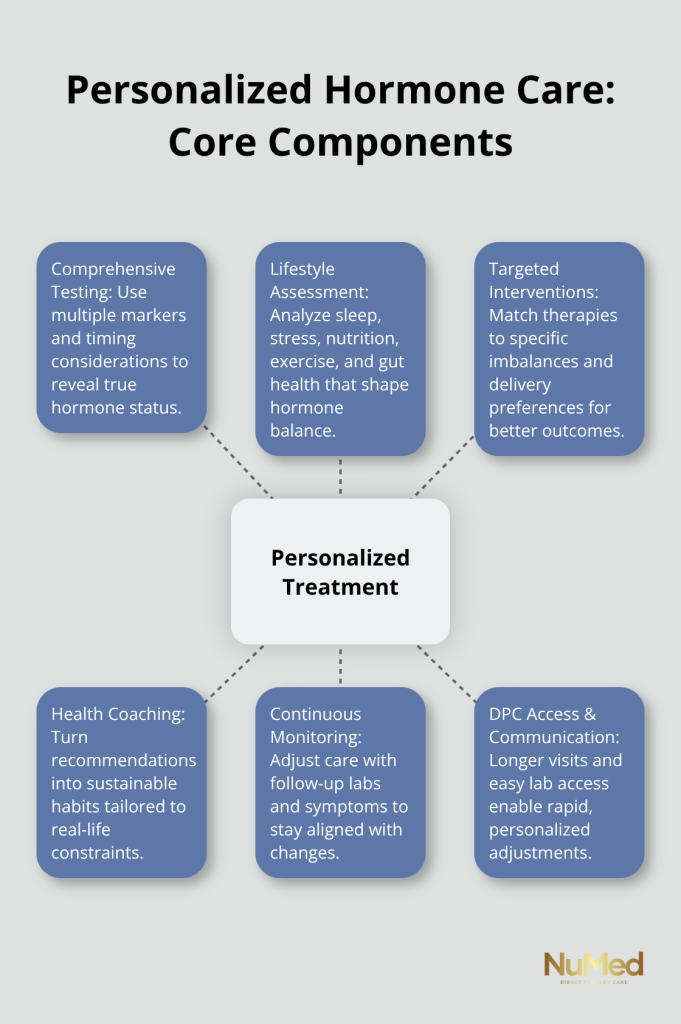
How Personalized Treatment Actually Works in Practice
Functional Medicine Examines Systems, Not Symptoms
Functional medicine forms the foundation of effective hormone optimization because it uses testing to identify early imbalances rather than treating isolated symptoms. This approach investigates nutrition status, sleep quality, stress resilience, gut function, and exercise patterns as integral parts of hormone health. A patient experiencing fatigue and weight gain receives an assessment of vitamin D levels, thyroid antibodies, cortisol patterns, insulin sensitivity, and inflammatory markers rather than a generic fatigue diagnosis. The International Menopause Society White Paper from 2024 reinforces that individualized hormone therapy decisions depend on a comprehensive assessment of your specific symptoms, lab values, and medical history rather than age-based protocols.
Functional medicine explicitly asks what your body needs to produce hormones optimally, then removes barriers and supplies missing nutrients. If your labs show vitamin D deficiency, supplementation becomes part of your plan because low vitamin D impairs testosterone production and estrogen metabolism. If sleep assessment reveals you’re averaging six hours nightly, sleep optimization becomes a priority because insufficient sleep reduces testosterone by up to fifteen percent the next day, according to sleep research.
Stress Management Prevents Hormonal Cascade
If stress patterns show elevated morning cortisol, your treatment includes stress management techniques like meditation or short breathing breaks rather than assuming medication alone will solve the problem. Chronic stress elevates cortisol, which suppresses thyroid function and testosterone while increasing appetite and fat storage around the abdomen. This systematic approach prevents the common scenario where patients receive hormone therapy while continuing behaviors that perpetuate imbalance.
Health Coaching Translates Understanding Into Action
Health coaching translates this understanding into sustainable action because hormonal symptoms create powerful psychological barriers to change. A woman experiencing severe hot flashes struggles with motivation to exercise, yet strength training naturally raises testosterone and supports fat loss that improves hormone metabolism. A man with low energy finds it difficult to prioritize sleep when work demands feel urgent, yet sleep represents the single most powerful lever for testosterone production.
Coaching helps you identify which changes will have the greatest impact on your specific situation, then removes obstacles to implementation rather than relying on willpower. Your coach works with you to build habits that stick, addressing the real barriers you face rather than offering generic advice that ignores your circumstances.
Continuous Monitoring Adjusts Treatment Over Time
Monitoring progress through regular follow-up appointments and repeat labs every three to six months allows your provider to adjust treatment as your body responds. If testosterone therapy causes elevated hematocrit or blood pressure, dosing is adjusted immediately rather than waiting months for an annual appointment. If lifestyle changes improve your symptoms but labs show a persistent imbalance, treatment intensifies or shifts. If hormone replacement therapy produces side effects, your provider switches delivery methods or adjusts dosing rather than dismissing your concerns. This continuous feedback loop transforms healthcare from a static prescription into a dynamic partnership where treatment evolves with your needs.
Final Thoughts
Hormone imbalance demands individualized care because your body’s chemistry is uniquely yours. Generic protocols fail because they ignore the specific combination of factors driving your symptoms-whether that’s sleep deprivation, stress patterns, nutritional gaps, or actual hormone deficiency. Effective personalized treatment for hormone imbalance requires testing that reveals your personal hormonal picture, lifestyle assessment that identifies what’s actually causing your imbalance, and ongoing adjustment as your body responds.
Direct Primary Care fundamentally changes what’s possible in hormone treatment by providing longer appointments where your provider understands your complete health picture, easy access to comprehensive lab testing without insurance delays, and ongoing communication through phone, email, or secure messaging. You receive transparent pricing upfront, which eliminates surprise bills and allows you to make informed decisions about testing and treatment. Most importantly, DPC creates continuity-your provider knows your history, your goals, and your response to previous interventions, so adjustments happen quickly rather than waiting months between appointments.
If fatigue, mood swings, weight gain, or other hormonal symptoms affect your quality of life, personalized treatment begins with assessment. Visit NuMed DPC to learn how our approach to hormone health differs from standard care and to schedule a consultation with a provider who will take time to understand your unique situation.
















