Most patients come to us frustrated. They’ve tried treating symptoms for years without getting better.
Functional medicine protocols work differently. Instead of masking what’s wrong, we identify and fix the root causes driving your health problems. At NuMed DPC, we’ve seen this approach transform outcomes that conventional care missed.
Why Conventional Care Falls Short for Chronic Illness
Most patients arrive frustrated. They’ve spent years treating symptoms without improvement. Chronic conditions affect about six in ten U.S. adults, and most cycle through appointments where doctors address isolated problems. Your blood pressure receives one medication. Your fatigue receives another. Your digestive problems get labeled as IBS and sent home with dietary suggestions that rarely work. The system doesn’t ask why these problems exist-it manages them individually, which is why so many people plateau and never fully recover.
Functional medicine protocols flip this approach entirely. Instead of asking what disease you have, we ask what caused the disease to develop. This distinction matters enormously. Conventional diagnostics rely primarily on standard blood tests and imaging to detect disease after symptoms appear, meaning you’re already significantly unwell before treatment begins. Functional medicine uses comprehensive diagnostics, including gut health tests, hormone panels, nutrient analyses, and, when clinically justified, genetic screening to detect imbalances early and identify the actual drivers of your symptoms.
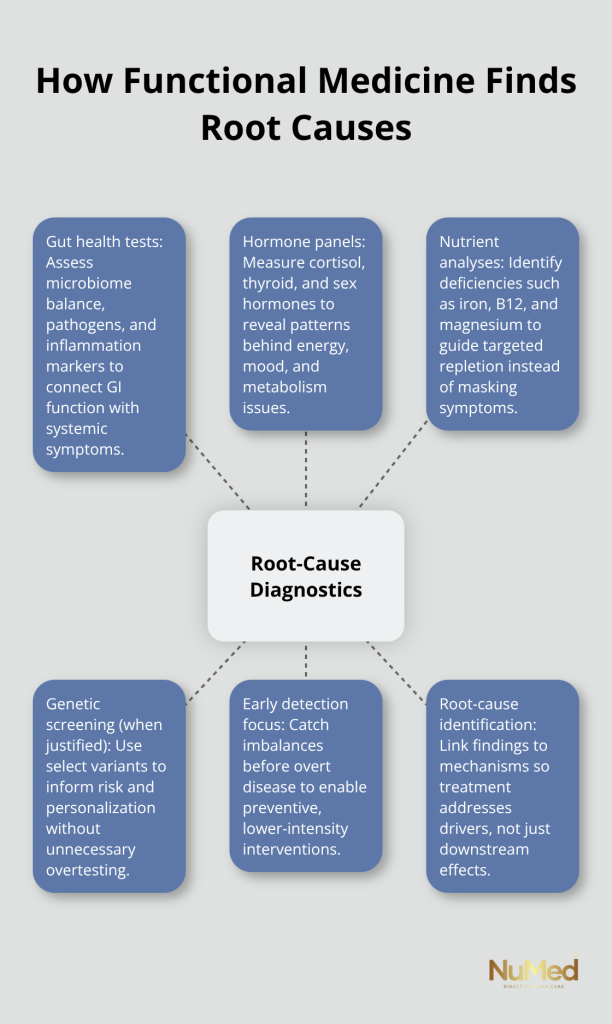
What Standard Testing Misses
A patient with fatigue, brain fog, and joint pain might have conventional tests come back normal, yet a functional medicine assessment reveals dysbiosis in the gut, magnesium deficiency, and blood sugar dysregulation that conventional testing never checked. These aren’t rare findings. The functional medicine timeline maps your health history from prenatal exposures through present-day symptoms to reveal long-term patterns that explain why your body struggles now. This approach demands personalized interventions because your root causes are unique to your genetics, environment, and life history. Someone else’s autoimmune protocol won’t fix your autoimmune condition because the triggers and mediators driving inflammation differ. The ATM model-Antecedents, Triggers, and Mediators-organizes this complexity by mapping long-term influences like childhood infections or environmental exposures, the specific events that activated your illness, and the ongoing contributors keeping you stuck. Treatment then targets what’s actually broken rather than what’s easiest to prescribe.
How Testing Reveals Root Causes
Standard blood panels show whether you have a disease. Functional medicine testing shows why you’re heading toward disease. A patient with elevated fasting glucose and insulin resistance might receive a pre-diabetes diagnosis conventionally and be prescribed metformin. Functional medicine assessment reveals that poor sleep quality drives cortisol dysregulation, which drives insulin resistance, which worsens from undiagnosed food sensitivities in their diet. The protocol then addresses sleep optimization, stress management, and elimination of trigger foods-interventions that conventional care rarely explores because they fall outside the standard disease-treatment framework. The functional medicine matrix organizes data across body systems, including digestion, immune function, energy production, detoxification, circulation, communication (nervous system), and structural integrity, with lifestyle factors at the center. This systems-based view prevents the fragmentation that plagues conventional care.
Integration Without Abandonment
Functional medicine is not a replacement for medicine. Functional medicine integrates with conventional care because both serve distinct and valuable purposes. Conventional medicine excels in acute medical care; infections need antibiotics, injuries need surgery, and chest pain needs emergency intervention. Functional medicine excels at chronic illness prevention and reversal, where lifestyle-first interventions prioritizing nutrition, movement, sleep, stress management, relationships, and purpose actually work when given time and proper support. Your functional medicine practitioner should be licensed (MD or DO preferred, as credentials matter significantly), should collaborate with your conventional doctors rather than compete with them, and should never ask you to abandon necessary medications without careful monitoring and plan adjustment. A hybrid approach combining both systems maximizes safety and outcomes.
Why Time Investment Matters
Initial functional medicine visits typically require 60 to 90 minutes to build a comprehensive, individualized plan-a stark contrast to the 10 to 15-minute conventional appointment where lifestyle discussion rarely happens. This time investment is not a luxury; it’s a necessity. Understanding how your genetics, environment, and daily choices interact to create your health problems takes conversation, investigation, and collaborative planning. The depth of assessment directly determines the quality of your protocol. A practitioner who spends 90 minutes understanding your complete history will identify patterns that a 15-minute visit cannot possibly reveal. This foundation shapes everything that follows in your treatment plan.
Implementing Your Protocol the Right Way
Building an effective functional medicine protocol requires three critical phases that most patients skip or rush through, which explains why they fail. The assessment phase determines everything downstream, and this is where most conventional practitioners fall short. Practitioners must spend substantial time gathering your complete health timeline, not just your current symptoms. This means understanding prenatal exposures, childhood infections, environmental toxins, dietary patterns across decades, stress history, sleep quality, relationships, and work satisfaction. The functional medicine timeline reveals patterns that explain your current state. A patient with autoimmune thyroiditis might discover that their condition emerged following a severe infection ten years ago, combined with chronic sleep deprivation from shift work, plus undiagnosed celiac disease that damaged their gut barrier. Standard testing would have flagged the thyroid antibodies. Functional assessment reveals why the autoimmune response was activated. This distinction transforms treatment.

Assessment Reveals What Standard Testing Misses
Testing must be selective and clinically indicated rather than reflexive. Practitioners order a comprehensive stool analysis when digestive symptoms or autoimmune conditions suggest gut dysfunction, because dysbiosis directly correlates with systemic inflammation and immune dysregulation. They assess nutrient status through appropriate labs when dietary intake appears inadequate or absorption is compromised. They evaluate hormone panels when fatigue, mood changes, or metabolic dysfunction suggest endocrine involvement. Each test serves a specific purpose within your unique clinical picture rather than following a standardized panel that wastes money and creates false positives. This targeted approach prevents the fragmentation that plagues conventional care and ensures that every assessment tool contributes directly to your personalized protocol.
Intervention Design Requires Ruthless Prioritization
Once assessment reveals root causes, intervention must target the highest-impact factors first. This is where practitioners diverge significantly from effective care. A patient with metabolic syndrome, dysbiosis, and chronic stress needs a prioritized protocol, not a simultaneous overhaul of diet, supplements, sleep, exercise, and stress management. Lifestyle-first interventions prioritize nutrition, movement, sleep, stress reduction, relationships, and purpose before supplements become relevant. Practitioners start with the intervention that addresses the greatest driver of dysfunction. If poor sleep quality drives 60 percent of your fatigue and metabolic dysfunction, sleep optimization becomes phase one. Specific strategies matter more than vague recommendations. Instead of telling you to sleep better, practitioners identify whether your sleep disruption stems from cortisol dysregulation (requiring evening magnesium and reduced blue light exposure), from sleep apnea (requiring testing and treatment), or from caffeine sensitivity (requiring elimination timing adjustments). These require different interventions. Supplements enter the picture only after lifestyle foundations are strengthened, and they target specific deficiencies or support specific mechanisms. A magnesium glycinate supplement addresses documented magnesium depletion or supports sleep quality when combined with sleep hygiene changes. Targeted support differs fundamentally from the supplement-heavy protocols that practitioners use to justify expensive product lines.
Gradual Implementation Prevents Overwhelm
Practitioners must implement changes gradually to prevent overwhelm and improve adherence. Asking someone to simultaneously change their diet, start an exercise program, restructure their sleep schedule, and manage stress sets them up for failure. A realistic first month might focus on eliminating one primary food trigger while establishing a consistent bedtime. Month two adds movement. Month three addresses stress management. This sequencing respects the reality of behavioral change rather than expecting transformation overnight. Practitioners who rush this phase watch patients abandon protocols within weeks, which explains why so many functional medicine attempts fail despite sound clinical reasoning.
Monitoring Determines Protocol Success
The final phase separates successful protocols from abandoned ones. Most practitioners establish a plan, then see patients infrequently without structured follow-up. Effective practitioners track progress through multiple measures simultaneously. Lab testing, when clinically indicated, reveals whether interventions correct underlying imbalances. A patient addressing dysbiosis might repeat stool analysis after three months of dietary modification and targeted probiotics to confirm microbial diversity has improved. Regular symptom check-ins using standardized measures like PROMIS tools provide objective data beyond subjective reporting. These tools quantify fatigue, physical function, and emotional well-being changes across time. Patient-reported outcomes matter because they reflect real-world experience. Monitoring appointments occur more frequently during protocol implementation, typically every 4 to 6 weeks initially, then extend to 8 to 12 weeks once stability emerges. This cadence provides accountability and allows protocol adjustment before patients lose motivation. Clear, measurable goals established at the beginning guide evaluation. Instead of the vague goal of feeling better, specific targets might include reducing fatigue severity from 7/10 to 4/10 within three months, improving fasting glucose from 110 to 95 mg/dL, or restoring energy sufficient to exercise four times weekly. Measurable objectives sustain engagement because progress becomes visible and quantifiable rather than hoped-for and uncertain. This structured approach to monitoring transforms what could be a passive experience into an active partnership where both practitioner and patient track real progress toward defined health outcomes.
Three Protocols That Actually Work
Effective functional medicine protocols target specific mechanisms rather than follow standardized templates. The difference between protocols that work and those that fail lies in how practitioners apply them to individual biochemistry. A food elimination protocol that works brilliantly for one patient produces zero results for another because their root causes differ. Practitioners must diagnose the actual problem before selecting the intervention, not the reverse. The most common mistake practitioners make is implementing elimination diets without first understanding whether food sensitivities drive the patient’s symptoms or whether dysbiosis, hormonal dysfunction, or nutrient malabsorption represents the true culprit. Testing reveals this distinction.
Patients with elevated zonulin levels, indicating intestinal permeability, respond dramatically to elimination diets paired with gut-healing nutrients like L-glutamine and collagen peptides because their barrier dysfunction drives systemic inflammation. Patients with normal intestinal permeability but dysbiosis require different intervention: they need fermented foods, specific-carbohydrate diets, and targeted prebiotics that feed beneficial bacteria rather than restriction alone. This targeted approach means some patients achieve complete symptom resolution within six to eight weeks of protocol implementation, while others require three to four months because their underlying mechanisms differ. The functional medicine matrix organizes these distinctions by mapping which body system requires intervention, preventing the one-size-fits-all mentality that ruins protocols.
Which Foods Actually Need Removal
Elimination diets work only when practitioners identify which specific foods trigger each patient’s symptoms. Generic elimination protocols removing gluten, dairy, and processed foods help some patients but waste time for others whose sensitivities lie elsewhere. Comprehensive stool analysis reveals dysbiosis patterns that indicate whether fermented foods will help or harm. A patient with small intestinal bacterial overgrowth worsens on high-fiber diets and fermented foods because excess bacteria ferment these compounds, producing gas and bloating that mimic food intolerance. The same foods benefit a patient with insufficient beneficial bacteria.
Practitioners must order appropriate testing first, then design food protocols matching the patient’s specific dysbiosis profile. Nutritional intervention extends beyond removal to targeted nutrient repletion. A patient with documented iron deficiency anemia requires different support than someone with B12 deficiency, yet both present with fatigue. Iron supplementation helps one and does nothing for the other. Magnesium deficiency drives muscle tension, sleep disruption, and metabolic dysfunction simultaneously, yet practitioners often address these symptoms separately with different medications rather than correcting the underlying deficiency. Targeted nutrient repletion addresses root causes that elimination diets alone cannot fix.
Practitioners assess nutrient status through comprehensive metabolic panels and specialized testing when indicated, then supplement strategically to restore function. This specificity transforms protocols from generic recommendations into powerful interventions matched to actual biochemistry.
Microbiome Recovery Requires Patience and Precision
Gut health restoration demands understanding that dysbiosis does not resolve through supplements alone or dietary changes without addressing what caused the dysbiosis initially. Prolonged antibiotic use, chronic stress, poor sleep quality, and processed food consumption all create dysbiotic patterns, and interventions must address the actual cause. A patient whose dysbiosis stems from antibiotic exposure responds to probiotic supplementation and fermented foods, while someone whose dysbiosis results from unmanaged stress requires concurrent stress management because dysbiosis recurs without addressing the stressor.
Microbiome rebalancing typically requires three to six months minimum because bacterial populations shift slowly. Practitioners who promise faster results oversell the pace of biological change. Effective protocols include dietary modifications that increase plant diversity to at least 30 different plant foods weekly, targeted probiotic supplementation matched to the patient’s dysbiosis pattern, and stress management because the gut-brain axis means cortisol dysregulation perpetuates dysbiosis regardless of dietary changes. Repeated testing at three and six months tracks whether microbial diversity improved and whether pathogenic bacteria decreased.

This monitoring prevents practitioners from maintaining ineffective interventions beyond the point of benefit.
Hormone Optimization Restores Metabolic Function
Hormone optimization addresses metabolic dysfunction that diet and lifestyle changes alone cannot resolve. Thyroid dysfunction, cortisol dysregulation, and sex hormone imbalances drive metabolic rate, inflammation, energy production, and body composition simultaneously. Standard thyroid testing, which checks only TSH, misses many hormone-driven problems because TSH remains normal while free T3 and free T4 decline, producing fatigue and weight gain that patients suffer through for years. Comprehensive hormone panels reveal these imbalances, and targeted interventions restore function.
A patient with elevated cortisol throughout the day requires different support than someone with flattened cortisol patterns, yet both present with fatigue. One needs stress management and cortisol-lowering supplements like phosphatidylserine, while the other requires adaptogenic support to raise baseline cortisol. This precision prevents wasted supplementation and delivers actual metabolic improvement.
Final Thoughts
Functional medicine protocols work when practitioners apply them with precision and patients commit to the process. The difference between success and failure lies not in the protocols themselves but in how carefully they match individual biochemistry and how consistently they address root causes rather than symptoms. We at NuMed DPC have watched patients recover from conditions that conventional medicine labeled permanent, with fatigue resolving, autoimmune markers improving, and metabolic dysfunction reversing because functional medicine protocols target what actually broke rather than what’s easiest to prescribe.
Working with qualified practitioners matters enormously-your practitioner must hold appropriate licensure (typically MD or DO credentials) and must demonstrate willingness to collaborate with your conventional doctors rather than compete with them. They should spend substantial time understanding your complete health history, order testing strategically rather than reflexively, and implement changes gradually to prevent overwhelm. Practitioners who rush assessment, oversell supplements, or promise unrealistic timelines undermine the entire approach, so verify credentials, ask for evidence supporting recommended interventions, and ensure your practitioner tracks measurable progress through regular monitoring.
Long-term health outcomes depend on sustained commitment beyond the initial protocol phase, as patients who achieve dramatic improvements within three to six months often plateau if they abandon the lifestyle changes that created improvement. Sleep quality, stress management, nutritional choices, and movement patterns require ongoing attention, not as a burden but as freedom from the medication treadmill that conventional care offers. If you’re ready to address root causes rather than manage symptoms indefinitely, explore how NuMed Direct Primary Care applies functional medicine to your unique health situation.