At NuMed DPC, we’ve found that most people never discover their root causes because they’re treated with a one-size-fits-all approach. This guide walks you through practical strategies and personalized testing that can help you regain hormonal stability.
Understanding Hormonal Imbalance and Its Symptoms
What Your Hormonal Symptoms Actually Mean
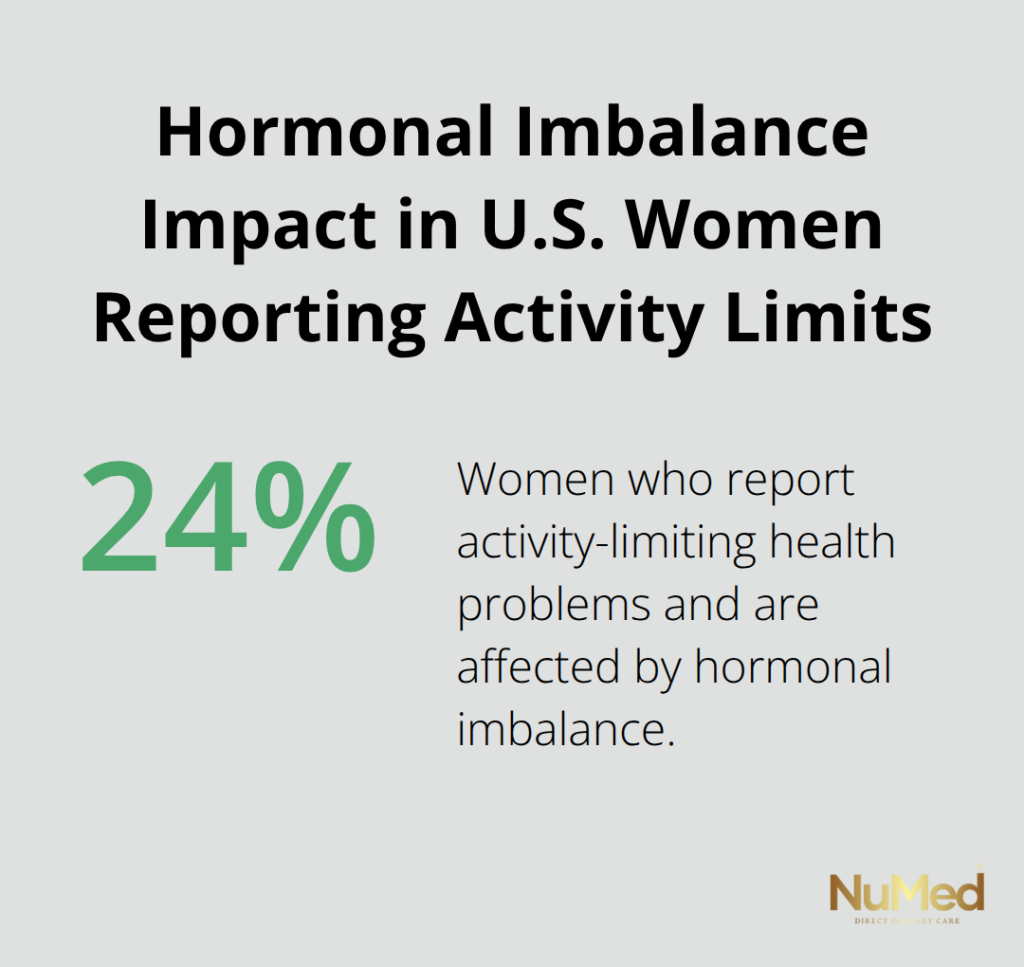
Fatigue that doesn’t improve with sleep, unexplained weight gain around the midsection, mood swings that feel disconnected from your circumstances, and skin breakouts that persist into adulthood signal that something in your endocrine system needs attention. These aren’t character flaws or signs you’re not trying hard enough. Hormonal imbalance affects roughly 24% of women who report health problems limiting daily activities, yet many people spend years treating symptoms without understanding what’s actually wrong.
The Cleveland Clinic identifies common signs, including fatigue, mood swings, irregular periods or PMS, weight changes, acne or hair loss, poor sleep, and low libido. What makes hormonal imbalance particularly tricky is that these symptoms overlap with dozens of other conditions-depression, thyroid disorders, sleep apnea, nutritional deficiencies-which is why multiple doctor visits often leave you without real answers. The endocrine system doesn’t work in isolation; it’s woven into every metabolic process, which means a single hormone imbalance creates a cascade of problems across your body.
How Your Daily Habits Rewire Your Hormones
Your hormones respond immediately to what you eat, how much you sleep, your stress load, and even your exercise intensity. The Cleveland Clinic notes that the endocrine system is highly sensitive to chronic stress, poor nutrition, environmental toxins, and disrupted sleep, meaning small disruptions compound quickly into measurable imbalances.
Cortisol suppresses progesterone production and disrupts your sleep-wake cycle further, creating a feedback loop that’s difficult to escape without intervention. Insulin resistance develops when refined carbohydrates and processed foods dominate your diet, and declining insulin sensitivity is particularly pronounced during perimenopause, when estrogen loss alters how your liver and pancreas handle glucose.
Your reproductive hormones-estrogen, progesterone, testosterone, LH, and FSH-depend on adequate overall calorie intake, unsaturated fats for hormone synthesis, and sufficient protein, which is why restrictive dieting often backfires spectacularly. Physical inactivity accelerates hormonal decline; the Study of Women’s Health Across the Nation shows that about 6,000 steps per day is associated with reduced cardiovascular and metabolic risk in middle-aged women, while sedentary habits accelerate weight gain and insulin resistance during the menopausal transition.
Why Testing Reveals What Symptoms Cannot
Symptoms alone cannot tell you whether your fatigue stems from low thyroid function, elevated cortisol, iron deficiency, or progesterone insufficiency-conditions that require completely different treatment approaches. Functional medicine testing goes beyond standard blood work to measure specific hormone levels, insulin resistance markers like HOMA-IR, fasting glucose, lipid panels, and waist circumference, which together paint a clear picture of your metabolic health.
A structured metabolic screening approach works best when you implement it as irregular cycles begin, with follow-ups every six months to track changes and catch problems early. The difference between guessing and testing is substantial: a woman experiencing weight gain and fatigue might assume she needs to eat less and exercise more, when in fact her progesterone has dropped 40%, and her cortisol is elevated, making calorie restriction and intense workouts counterproductive. Testing transforms vague symptoms into actionable data, allowing you and your practitioner to target interventions where they’ll actually work rather than applying generic advice that misses the real problem entirely. This is where personalized approaches become essential-and where understanding your individual hormonal profile opens the door to real solutions.
What Actually Works to Balance Hormones
Nutrition as Your Hormonal Foundation
Nutrition forms the foundation of hormonal stability because food directly influences how your body produces, metabolizes, and clears hormones. Cruciferous vegetables like broccoli, cauliflower, and Brussels sprouts contain compounds called indole-3-carbinol and sulforaphane that support estrogen metabolism and liver detoxification. Light steaming preserves these nutrients better than heavy cooking.
Wild-caught fatty fish, including salmon, mackerel, and sardines, provide EPA and DHA omega-3s that modulate inflammation and improve how your cells respond to hormones; Harvard T.H. Chan School of Public Health recommends two servings weekly as a clinically supported target. Soluble fiber from oats, lentils, apples, and chia seeds binds estrogen in your gut and stabilizes insulin levels, which the National Library of Medicine confirms is essential for clearing excess hormones and preventing blood sugar swings that trigger cortisol spikes.
Fermented foods like kimchi, sauerkraut, and kefir promote gut microbial diversity, which directly supports estrogen metabolism and overall endocrine function, according to Harvard Health Blog research. Healthy fats from avocados, nuts, seeds, and cold-pressed olive oil support steroid hormone synthesis at the cellular level. Refined sugars, heavily processed foods, alcohol, and excessive caffeine actively disrupt cortisol, insulin, and estrogen levels, making them worth eliminating rather than moderating.
Sleep Quality and Circadian Rhythm Regulation
Sleep quality matters more than sleep quantity for hormonal balance because irregular sleep patterns destabilize your circadian rhythm and suppress melatonin production. Exposure to morning sunlight within the first hour of waking synchronizes your internal clock and downstream hormone regulation throughout the day.

A sleep sanctuary with complete darkness and white noise, if needed, creates the environment your body needs to produce adequate melatonin and maintain proper cortisol rhythms. Consistent bedtime and wake times anchor your endocrine system far more effectively than sleeping different hours on weekends.
Movement and Exercise Intensity Matter
Physical activity reduces insulin resistance and cortisol when structured appropriately. Intense exercise actually elevates cortisol acutely, so pairing moderate-intensity movement like walking with resistance training preserves lean muscle mass during hormonal transitions without triggering chronic stress hormone elevation. This balanced approach prevents the counterproductive effects of overtraining while still supporting metabolic health.
Stress Management and Hormonal Recovery
Stress management directly impacts your HPA axis, the communication pathway between your brain and adrenal glands that controls cortisol output. Chronic psychological stress suppresses progesterone while elevating cortisol, creating the fatigue and mood instability you experience.
Omega-3-rich diets, legumes, produce, and whole grains provide antioxidants and anti-inflammatory compounds that actively reduce cortisol levels, making these foods doubly valuable for stress resilience. When you address stress through both dietary support and behavioral practices, your hormonal system begins to stabilize more rapidly than through nutrition alone.
Understanding these foundational strategies positions you to make immediate changes, yet the real transformation happens when you identify which specific hormonal imbalances are actually driving your symptoms. This is where testing and personalized assessment become the bridge between general knowledge and targeted action.
Why Generic Hormone Advice Fails You
The reason most people struggle with hormonal balance is that standard medical care treats hormones as isolated problems rather than symptoms of your specific metabolic environment. A woman with irregular periods might receive birth control pills without any investigation into whether her problem stems from insulin resistance, chronic stress, nutrient deficiency, or estrogen dominance-three completely different root causes that require opposite treatment strategies. Generic solutions fail because they ignore the fact that your hormonal imbalance reflects your individual genetics, stress history, dietary patterns, sleep quality, exercise habits, and environmental exposures. What works brilliantly for one person can make another person’s symptoms worse, which is why the nutrition and lifestyle strategies from the previous section only deliver results when they match your actual hormonal profile.
Testing Transforms Guesswork Into Precision
Functional medicine testing reveals the specific hormonal and metabolic markers that drive your symptoms, moving you from assumptions to measurable data. A comprehensive metabolic assessment includes fasting glucose and insulin levels to calculate HOMA-IR, a lipid panel showing how your body handles cholesterol and triglycerides, thyroid function tests including TSH and free T3 and T4, cortisol patterns across the day, reproductive hormone levels like estrogen, progesterone, and testosterone (depending on your cycle phase), and inflammatory markers like high-sensitivity C-reactive protein. For women in perimenopause, the Study of Women’s Health Across the Nation research shows that LDL cholesterol, total cholesterol, and triglycerides rise during late perimenopause while HDL quality worsens, making baseline testing essential to catch these shifts before they progress.
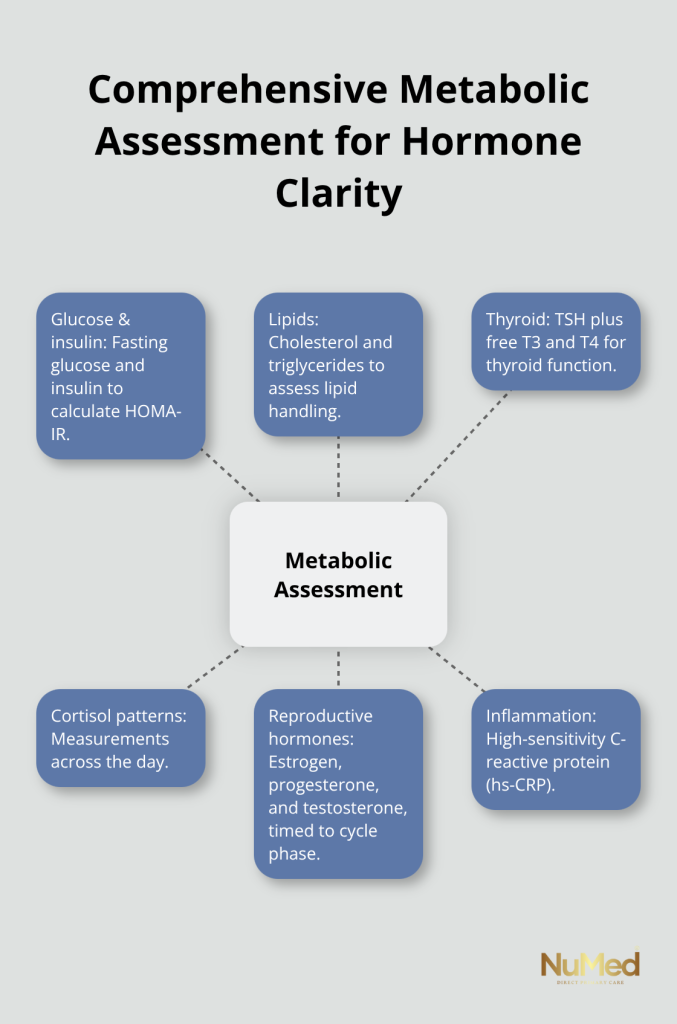
A structured metabolic screening approach implemented when irregular cycles begin, then repeated every six months, allows you and your practitioner to track whether your interventions actually work rather than relying on how you feel. Many conventional doctors order only TSH for thyroid screening, missing subclinical hypothyroidism and the free T3 suppression that drives fatigue and weight gain. A functional medicine practitioner orders the complete picture, recognizing that your hormonal system cannot be understood through isolated lab values.
Building a Personalized Treatment Plan That Sticks
Working with a practitioner who spends genuine time understanding your health history, stress patterns, sleep environment, digestive function, and exposure to toxins differs fundamentally from a 15-minute appointment focused on symptom management. Direct Primary Care practices provide the time and access needed for this deeper assessment, including initial visits of 30 to 90 minutes where your practitioner can explore how your hormones connect to your sleep, nutrition, stress, movement patterns, and gut health in a single coordinated plan. This comprehensive approach identifies why your cortisol remains elevated despite meditation attempts, or why increasing fiber intake has not resolved your estrogen clearance problems-often because a secondary factor like poor sleep quality or unmanaged food sensitivities blocks progress. Your practitioner then tailors specific interventions: perhaps you need adaptogenic herbs like ashwagandha to support your HPA axis function, targeted supplementation to address nutrient gaps identified through testing, or strategic timing of meals and exercise to optimize your circadian rhythm and insulin sensitivity. The critical difference is accountability-DPC models include ongoing messaging and same-day appointment access, enabling rapid adjustments to your hormone plan as your labs improve and symptoms shift. This continuous feedback loop prevents you from staying stuck on interventions that do not work and accelerates progress toward sustainable hormonal wellness.
Conclusion
Hormonal balance requires understanding your specific metabolic environment, identifying which hormonal imbalances drive your symptoms, and implementing targeted strategies that match your individual needs. Testing reveals your actual hormone levels, insulin sensitivity, thyroid function, and inflammatory markers rather than leaving you to guess based on symptoms that could indicate dozens of different problems. A woman experiencing irregular periods and weight gain needs to know whether her issue stems from insulin resistance, progesterone deficiency, elevated cortisol, or thyroid dysfunction before any intervention can work.
Working with a practitioner who takes time to understand your complete health picture transforms your ability to achieve results. At NuMed DPC, we focus on preventing illness by addressing root causes through personalized connections between patient and practitioner. Our direct primary care model provides the extended visits, functional medicine testing, and ongoing access needed to identify what’s actually driving your hormonal imbalance and adjust your treatment plan as your body responds.
The natural way to get hormones in balance starts when you stop applying generic solutions and address your individual needs instead. Schedule a consultation to discuss your symptoms, health history, and goals with a practitioner who will order comprehensive testing and develop a plan tailored to your hormonal profile. Sustainable hormonal wellness begins with this personalized approach.