Hormonal imbalances affect millions of people, causing fatigue, weight fluctuations, mood changes, and sleep disruption. The good news is that natural ways to balance hormones often start with simple, evidence-based changes to diet, sleep, and stress management.
At NuMed DPC, we’ve seen firsthand how targeted lifestyle modifications can restore hormonal function without relying solely on medication. This guide walks you through the practical strategies that actually work.
What Your Hormones Are Actually Telling You
Your body produces over 50 hormones daily, but five dominate your overall health: cortisol, estrogen, progesterone, insulin, and thyroid hormones. When these go out of balance, you notice it immediately. Fatigue hits harder than it should, weight creeps on despite eating the same, mood swings intensify, and sleep becomes elusive. Chronic stress, poor nutrition, environmental toxins, disrupted sleep, and underlying medical conditions trigger these imbalances because your endocrine system is exquisitely sensitive to stressors. Most people ignore early warning signs until symptoms compound. Irregular periods, persistent acne, low libido, and unexplained irritability are not personality quirks or normal aging-they’re your body flagging a problem that responds well to intervention.
Cortisol Runs the Show
Cortisol, your primary stress hormone, naturally rises in the morning and falls by evening. Elevated cortisol throughout the day causes fatigue, weight gain around the midsection, weakened immunity, and poor sleep quality. Modern life keeps cortisol perpetually high through work stress, poor sleep, excessive caffeine, and skipped meals. You cannot eliminate stress, but you can prevent constant elevation through specific actions. Eating protein and fat at breakfast within two hours of waking stabilizes cortisol and prevents the afternoon crash. Limiting caffeine to before noon protects your evening cortisol drop, which is essential for sleep onset. Regular moderate exercise reduces cortisol, though intense workouts without adequate recovery actually raise it further. Sleep deprivation elevates cortisol the next day and disrupts the entire hormonal cascade.
Sex Hormones and Metabolic Health
Estrogen and progesterone regulate far more than menstrual cycles. They influence metabolism, bone density, mood, and cardiovascular health. Imbalances manifest as irregular periods, infertility, acne, brain fog, and depression. Adequate fiber intake directly supports estrogen clearance through the gut. Fiber-rich foods like oats, lentils, apples, and chia seeds bind excess estrogen for elimination. Healthy fats from avocados, nuts, seeds, and olive oil provide essential fatty acids required for steroid hormone synthesis. Undereating calories or fat, a common pattern in people trying to lose weight, actually suppresses sex hormone production. Testosterone, present in both men and women, supports muscle mass, bone strength, and sexual function. Low testosterone causes fatigue and reduced muscle recovery.
Thyroid Hormones Control Your Metabolism
Thyroid hormones T3, T4, and TSH regulate metabolism, energy, temperature regulation, and mood. Hypothyroidism, where thyroid function drops, causes weight gain, fatigue, cold sensitivity, and depression. The Endocrine Society emphasizes that adequate calories, including sufficient carbohydrates, are non-negotiable for thyroid health. Undereating suppresses T3 production within days. Iron, zinc, iodine, selenium, and vitamin B12 are essential cofactors for thyroid hormone synthesis and conversion. Iodized salt provides iodine, but many people avoid salt due to blood pressure concerns. Seaweed products like nori contain iodine without excess sodium. Brazil nuts deliver selenium. Just two nuts daily meet your requirement. Animal proteins, legumes, and whole grains supply iron and zinc. Vitamin B12 comes from animal products or fortified nutritional yeast. Testing TSH, free T4, and free T3 reveals whether your thyroid actually functions properly or whether symptoms stem from nutrient deficiencies or conversion problems in the liver and gut.
Moving Forward With Dietary Support
Understanding what your hormones signal about your health sets the stage for practical intervention. The next section covers the specific foods and nutrients that stabilize these five hormones and restore balance through evidence-based dietary choices.
Dietary Approaches to Support Hormonal Balance
Insulin stability forms the foundation of hormonal balance, yet most people structure meals in ways that spike and crash blood sugar repeatedly throughout the day. Eating carbohydrates alone at breakfast sends insulin surging, which then plummets two hours later, triggering fatigue, cravings, and stress hormone release to compensate. This pattern destroys hormone balance in nearly every patient who hasn’t addressed meal composition. The fix is mechanical: combine protein, fat, and fiber at every meal and significant snack.

Foods That Stabilize Blood Sugar and Insulin Levels
Protein triggers slower glucose absorption and stabilizes satiety hormones. Fat slows digestion further and provides the building blocks for steroid hormone synthesis. Fiber binds excess estrogen for elimination and moderates insulin response. A breakfast of two eggs with cheese and spinach on whole-grain toast, paired with half an avocado, delivers all three macronutrients and keeps insulin stable for four to five hours. Lunch built around grilled salmon with olive oil drizzled over roasted broccoli and quinoa follows the same principle.
The Cornell Food and Brand Lab research shows that people who eat protein at breakfast consume 441 fewer calories daily because satiety hormones function properly. Snacks matter equally. An apple with two tablespoons of almond butter, or a small handful of nuts with a piece of cheese, prevents the afternoon blood sugar crash that triggers cortisol spikes and cravings for refined carbohydrates.
Timing influences hormone production directly. Eating within two hours of waking, with adequate protein and fat, stabilizes cortisol and prevents the midday energy collapse. Skipping breakfast or eating only carbohydrates in the morning guarantees elevated cortisol throughout the day. Conversely, eating late in the evening disrupts melatonin production and sleep quality because glucose elevation suppresses melatonin synthesis.
Micronutrients Essential for Hormone Synthesis
Your body cannot manufacture hormones without specific cofactors, yet most people consume these micronutrients in insufficient quantities. Iron, zinc, iodine, selenium, and vitamin B12 are non-negotiable for thyroid hormone production and conversion. Two Brazil nuts daily provide your entire daily selenium requirement, which is essential for thyroid peroxidase enzyme function. Iodized salt remains the most reliable iodine source, though seaweed products like nori sheets offer iodine without sodium concerns.
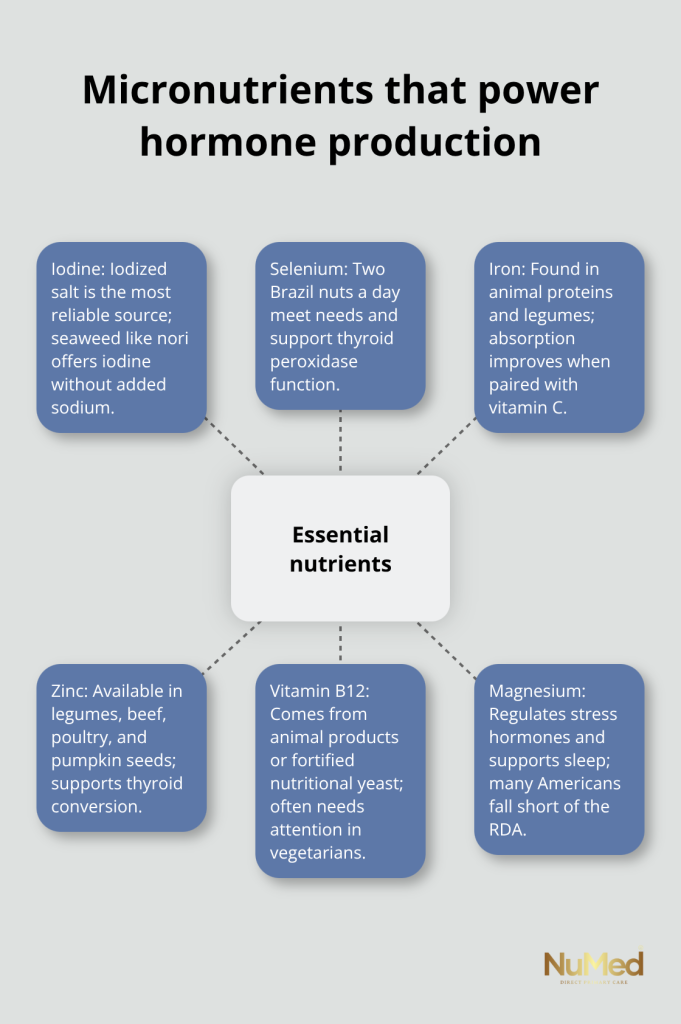
Zinc comes from legumes, beef, poultry, and pumpkin seeds, with the recommended daily allowance of 11 milligrams for men and 8 milligrams for women according to the National Institutes of Health. Iron absorption improves dramatically when consumed with vitamin C, so pair spinach or lentils with citrus, tomatoes, or bell peppers. Vitamin B12 exists only in animal products or fortified nutritional yeast, making supplementation or deliberate food choices necessary for vegetarians.
Magnesium regulates stress hormones through the HPA axis and supports sleep quality, yet 48% of Americans consume less than the recommended daily amount. Leafy greens, nuts, seeds, and whole grains supply magnesium, but supplementation at 200 to 300 milligrams daily often becomes necessary. Vitamin D influences sex hormone production and thyroid health, with the recommended daily allowance of 600 to 800 IU for adults, though many people require testing to determine if they need higher doses.
Fatty fish like salmon and mackerel deliver omega-3 fatty acids that reduce inflammation affecting hormone receptor sensitivity. Harvard T.H. Chan School of Public Health research supports consuming two servings of wild-caught fatty fish weekly to achieve the clinical target for EPA and DHA intake.
Timing and Macronutrient Ratios for Optimal Hormone Function
The proportion of protein, carbohydrate, and fat in your meals directly determines whether your hormones stabilize or destabilize. Protein should comprise 25 to 35 percent of total daily calories to support hormone production and maintain muscle mass, which declines with age and hormonal imbalance. Carbohydrates from whole grains, legumes, and vegetables should constitute 40 to 50 percent of calories, never eliminated despite trendy low-carb diets that suppress thyroid function within days. Fat should provide 25 to 35 percent of calories, with emphasis on unsaturated sources like olive oil, avocados, nuts, and seeds.
This ratio prevents the underfueling that suppresses estrogen and progesterone production in women and testosterone in men. A practical lunch structure that achieves this ratio includes four to six ounces of protein, one to two cups of vegetables prepared with one to two tablespoons of oil, and one-half to three-quarters cup of whole grains or starchy vegetables. Spacing meals four to five hours apart allows insulin to return to baseline and prevents the constant elevation that drives insulin resistance and metabolic dysfunction.
Skipping meals or practicing intermittent fasting without medical guidance backfires hormonally because caloric restriction triggers cortisol elevation and suppresses reproductive hormones. Women in particular experience menstrual irregularities and fertility problems when underfed, a pattern documented extensively in the literature on female athlete triad and eating disorders. Once you establish stable meal patterns and nutrient intake, your body responds by restoring hormonal function, but diet alone cannot address the full picture. Sleep quality, stress management, and movement patterns complete the hormonal restoration equation.
Sleep, Stress, and Movement Matter More Than You Think
Sleep deprivation obliterates hormone balance faster than any dietary mistake. The National Sleep Foundation recommends 7 to 9 hours nightly, yet 35 percent of American adults sleep less than 7 hours regularly. During sleep, your body restores cortisol rhythm, synthesizes growth hormone, consolidates metabolic memory, and clears metabolic waste through the glymphatic system.
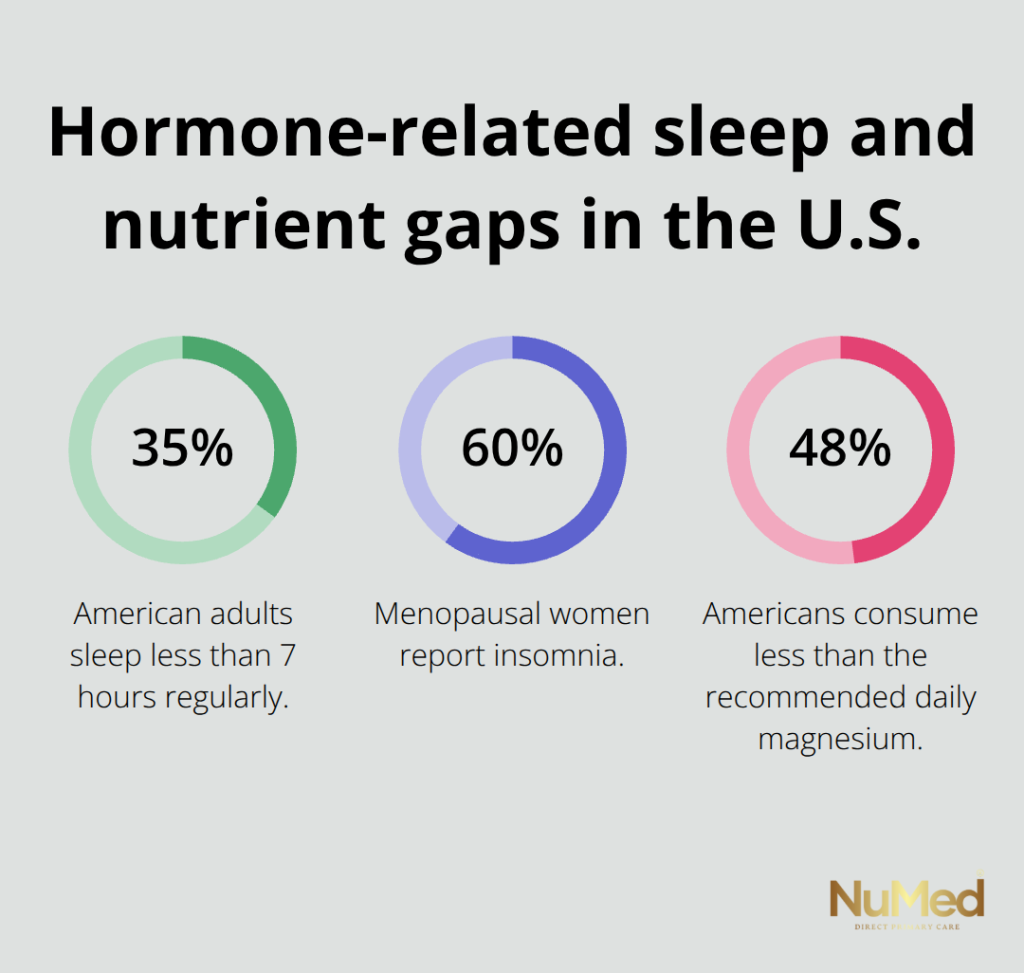
Insufficient sleep elevates evening cortisol, which suppresses melatonin production the following night, creating a downward spiral. Insomnia affects roughly 60 percent of menopausal women according to research published in Menopause Review, and sleep disruption raises evening cortisol while further suppressing estradiol.
Establish Consistent Sleep Patterns
The fix requires behavioral specificity, not generic sleep hygiene advice. Set a consistent bedtime and wake time seven days a week, even on weekends, because circadian misalignment from variable sleep schedules suppresses sex hormone production within days. Dim overhead lights two hours before bed since blue light suppresses melatonin synthesis. Keep your bedroom temperature between 60 and 67 degrees Fahrenheit because core body temperature must drop for sleep onset. If racing thoughts plague your nights, cognitive behavioral therapy for insomnia outperforms sleep medications for long-term results. Digital sleep tracking tools like Oura Ring or WHOOP provide objective data showing whether your sleep architecture actually includes sufficient deep and REM sleep, not just total hours. Most people discover they spend eight hours in bed but only six hours asleep, a distinction that changes treatment approach entirely.
Manage Stress Through Targeted Practices
Stress management directly regulates your nervous system and cortisol production, yet most people approach it as optional self-care rather than a medical necessity. Mindfulness-based stress reduction improves quality of life and reduces vasomotor symptoms in menopausal women, according to research from the Journal of Clinical Medicine. Cognitive behavioral therapy reduces insomnia severity by addressing thought patterns that trigger cortisol spikes at night. Practical implementation means selecting one stress management technique and practicing it consistently rather than sporadically sampling multiple methods.
Exercise With Balance and Intention
Thirty minutes of moderate aerobic exercise five days weekly reduces total and free estradiol levels more effectively in non-obese women, and when performed at higher intensity, according to research published in Cancer Epidemiology, Biomarkers and Prevention. Resistance training twice weekly improves bone mineral density at the lumbar spine and hips in postmenopausal women, with combined aerobic and resistance training producing superior results. Exercise also improves adipocyte metabolism and muscle regeneration during menopause. However, intense exercise without adequate recovery actually elevates cortisol further, so balance matters. Your body needs recovery days to restore hormonal function rather than perpetually taxing the stress response system.
Reduce Environmental Toxin Exposure
Environmental toxin exposure disrupts endocrine function through endocrine-disrupting chemicals like BPA and phthalates found in plastics, receipts, and cosmetics. Replace plastic food containers with glass, stainless steel, or ceramic alternatives. Choose personal care products certified by third-party organizations like the Environmental Working Group, since cosmetic regulations remain minimal. Limit alcohol consumption because excess disrupts estrogen and testosterone balance, according to NIH research. These modifications require deliberate choice and often involve replacing convenient habits with slightly more intentional alternatives, but the hormonal restoration they produce makes the effort worthwhile.
Final Thoughts
The natural ways to balance hormones outlined in this guide work because they address root causes rather than masking symptoms. Stabilizing blood sugar through proper meal composition, ensuring adequate sleep, managing stress intentionally, and moving your body with purpose create the conditions your endocrine system needs to function optimally. These changes compound over weeks and months, producing measurable improvements in energy, mood, sleep quality, and metabolic health.
Your body possesses a remarkable capacity to heal when given the right inputs. Hormonal imbalance did not develop overnight, and restoring balance requires patience and consistency rather than perfection. Missing one workout or eating a processed meal occasionally does not derail progress-what matters is the overall pattern of your choices across weeks and months.
Persistent symptoms despite implementing these strategies warrant professional evaluation, as thyroid dysfunction, PCOS, adrenal insufficiency, and other medical conditions require testing and sometimes medication alongside lifestyle modifications. Contact NuMed DPC to identify root causes of hormonal dysfunction through comprehensive lab assessment and personalized treatment plans that combine natural approaches with medical guidance when necessary.