Functional medicine takes a fundamentally different approach to healthcare than what most people experience. Instead of treating symptoms as isolated problems, practitioners search for the underlying causes of illness.
At NuMed DPC, we’ve seen firsthand how this approach resonates with patients seeking real answers. The question isn’t whether functional medicine works-it’s whether it’s worth it for your specific health situation.
How Functional Medicine Differs from Conventional Care
Conventional medicine excels at treating acute infections, injuries, and emergencies, but it struggles with chronic conditions because the system prioritizes quick visits and symptom suppression. A typical conventional appointment lasts 10 to 15 minutes, leaving little room to explore what caused your problem in the first place. Your doctor prescribes medication for high blood pressure, but nobody asks why your blood pressure climbed or whether stress, sleep deprivation, or inflammatory foods triggered it. The result is that you treat the symptom while the underlying driver continues to damage your health.
Functional medicine inverts this logic entirely. Instead of asking what drug matches your diagnosis, practitioners ask what imbalance or dysfunction created your symptoms. This matters because addressing root cause analysis in chronic disease management produces lasting improvement, not just temporary relief. A functional medicine practitioner might spend 60 to 90 minutes on your first visit, reviewing your complete health history, lifestyle, genetics, and environment. That extended time reveals patterns that conventional care misses. Someone with fatigue and brain fog might discover that poor sleep timing, insufficient protein intake, or undiagnosed food sensitivities are the real culprits, not a deficiency requiring supplements.
Where Diagnostic Testing Diverges
Conventional diagnostics rely on standard lab work like basic metabolic panels and cholesterol counts, which detect disease once it has already advanced. Functional medicine uses functional testing to identify imbalances before they become disease. Gut microbiome analysis, comprehensive hormone panels, nutritional markers, and inflammatory markers reveal dysfunction that standard labs ignore. You might have a normal cholesterol reading yet still have oxidative stress driving heart disease risk, something functional testing can uncover.

This testing-informed approach costs more upfront but prevents expensive interventions later. Insurance typically covers standard labs but not specialized functional testing, which is why costs become a real consideration.
The Relationship Model Changes Everything
Conventional medicine treats each visit as a transaction; functional medicine builds an ongoing relationship. Your functional medicine practitioner knows your goals, your barriers to change, and your response to previous interventions. This continuity means faster adjustments when something isn’t working and better support for behavior change. You have access between visits via messaging, same-day appointments when needed, and a practitioner who remembers your history without scrolling through charts. That relationship accountability accelerates progress because you’re not starting from scratch every visit, explaining your situation to someone who has never seen you before.
Why This Matters for Your Health Decisions
The differences between these two models shape what you can expect from your care. Conventional medicine offers rapid diagnosis and treatment for acute problems, but chronic conditions (autoimmune disease, digestive disorders, hormonal imbalance, persistent fatigue) require the kind of sustained attention and root-cause investigation that functional medicine provides. Understanding these distinctions helps you decide which approach fits your current health needs and which practitioner model will actually address what matters most to you.
Does Functional Medicine Deliver Real Results?
The evidence supporting functional medicine’s effectiveness in chronic disease management has grown substantially over the past decade. A 2023 study published in the AMA Network Open examined patients using the functional medicine model and found significant improvements in patient-reported health-related quality of life compared to standard care. Patients with autoimmune conditions, digestive disorders, hormonal imbalances, and chronic fatigue reported measurable improvements within 4 to 12 weeks when practitioners addressed root causes rather than symptoms alone. The Veterans Affairs Whole Health program integrates functional medicine principles into conventional VA care and has documented reduced hospitalizations and emergency department visits among participants who engaged with root-cause protocols. These aren’t theoretical outcomes-they represent actual healthcare utilization data from large patient populations.
What the Numbers Show About Real Patient Improvement
The timeline for results matters practically. Short-term gains typically emerge within the first 4 to 12 weeks and include better energy levels, steadier digestion, improved sleep quality, and more predictable daily functioning. Longer-term durable changes usually require 3 to 6 months or more, with the biggest returns coming from consistent implementation of fundamentals rather than expensive testing or supplement stacks. A functional medicine practitioner who focuses on protein and fiber targets, optimized sleep timing, light exposure, physical activity combining strength and steps, and stress management skills produces better outcomes than one who orders endless specialty labs without behavioral support.

Insurance data and patient satisfaction surveys consistently show that patients who stay engaged with functional medicine protocols for at least three months report higher satisfaction and lower repeat office visit frequencies compared to conventional-only care, suggesting that the initial investment of time and money yields downstream savings through prevention.
Cost Reality and Long-Term Financial Impact
Functional medicine visits and specialized testing cost more upfront, with first visits ranging from 500 to 1,500 dollars, depending on the practitioner and location, plus specialty labs that insurance typically does not cover. However, the long-term financial picture shifts when you factor in prevented complications. Patients with prediabetes who implement functional nutrition and lifestyle protocols avoid progression to type 2 diabetes, which costs the U.S. healthcare system over 327 billion dollars annually in direct and indirect expenses per CDC data. Someone who prevents even one hospitalization for an autoimmune flare or one emergency department visit for an acute digestive crisis has already offset the cost of functional medicine care. The model works best when you commit to the behavioral changes it recommends-if you pay for extended visits and specialty testing but ignore nutrition and sleep recommendations, the financial value disappears.
How Functional Medicine Compares to Conventional Spending
Conventional medicine often spreads costs across multiple specialists, repeat imaging, and medication adjustments that accumulate without addressing underlying dysfunction. Functional medicine concentrates on spending upfront on comprehensive assessment and testing, then reduces downstream costs through prevention and early intervention. A patient with chronic migraines might spend 2,000 dollars on a functional medicine evaluation and testing, discover that food sensitivities and magnesium deficiency drive the headaches, and then eliminate the need for preventive medications and emergency visits. That same patient in conventional care might spend 3,000 to 5,000 dollars annually on neurologist visits, imaging, and prescription medications without ever identifying the root cause. The financial advantage of functional medicine emerges over 12 to 24 months, not in the first month.
Who Sees the Biggest Return on Investment
Patients with multiple chronic conditions, those who have failed conventional treatment approaches, and individuals motivated to change their lifestyle habits see the strongest results and best financial returns. Someone with stable, well-controlled acute conditions may not need functional medicine’s depth. However, anyone managing autoimmune disease, persistent fatigue, hormonal imbalance, or metabolic dysfunction stands to benefit substantially from the root-cause investigation and personalized protocols that functional medicine provides. The investment pays off fastest for those who actively implement dietary changes, sleep optimization, stress reduction, and movement protocols rather than those who expect supplements or testing alone to solve their problems.
Understanding whether functional medicine delivers real results requires looking beyond individual testimonials to the actual data on patient outcomes, timelines, and financial impact. The evidence shows measurable improvements in quality of life, reduced healthcare utilization, and long-term cost savings for engaged patients. These findings raise an important practical question: how do you identify a qualified functional medicine practitioner who can deliver these results, and what should you expect to pay?
How to Find the Right Functional Medicine Practitioner
Finding a qualified functional medicine practitioner requires verification beyond credentials alone. The Institute for Functional Medicine maintains a searchable provider directory, but a listing does not guarantee competence or a good fit for your needs. Start by confirming the practitioner holds an MD or DO license, not just a PA or chiropractor credential, though some PAs and chiropractors can deliver solid functional care if properly trained. Check whether they completed the Institute for Functional Medicine’s certification program, which involves substantial postgraduate training in systems biology and root-cause assessment. However, certification alone does not tell you if someone will spend the time your case requires or align with your specific health goals. Read patient reviews on Google and Healthgrades, focusing on comments about appointment length, follow-up responsiveness, and whether practitioners actually addressed root causes or simply ordered expensive tests without behavioral support. Many functional medicine practitioners now offer 15-minute discovery calls at no charge, which lets you ask directly about their testing philosophy, how they handle insurance billing, and whether they coordinate with your conventional doctor. This conversation reveals whether they practice evidence-based functional medicine or chase every trendy specialty lab. Proximity and telemedicine access matter practically. If your practitioner is three hours away, you will not maintain the ongoing relationship that makes functional medicine effective. Many qualified practitioners now offer telehealth for follow-up visits, which reduces travel burden while preserving the continuity that drives results.
Insurance Coverage Creates Your Real Cost Picture
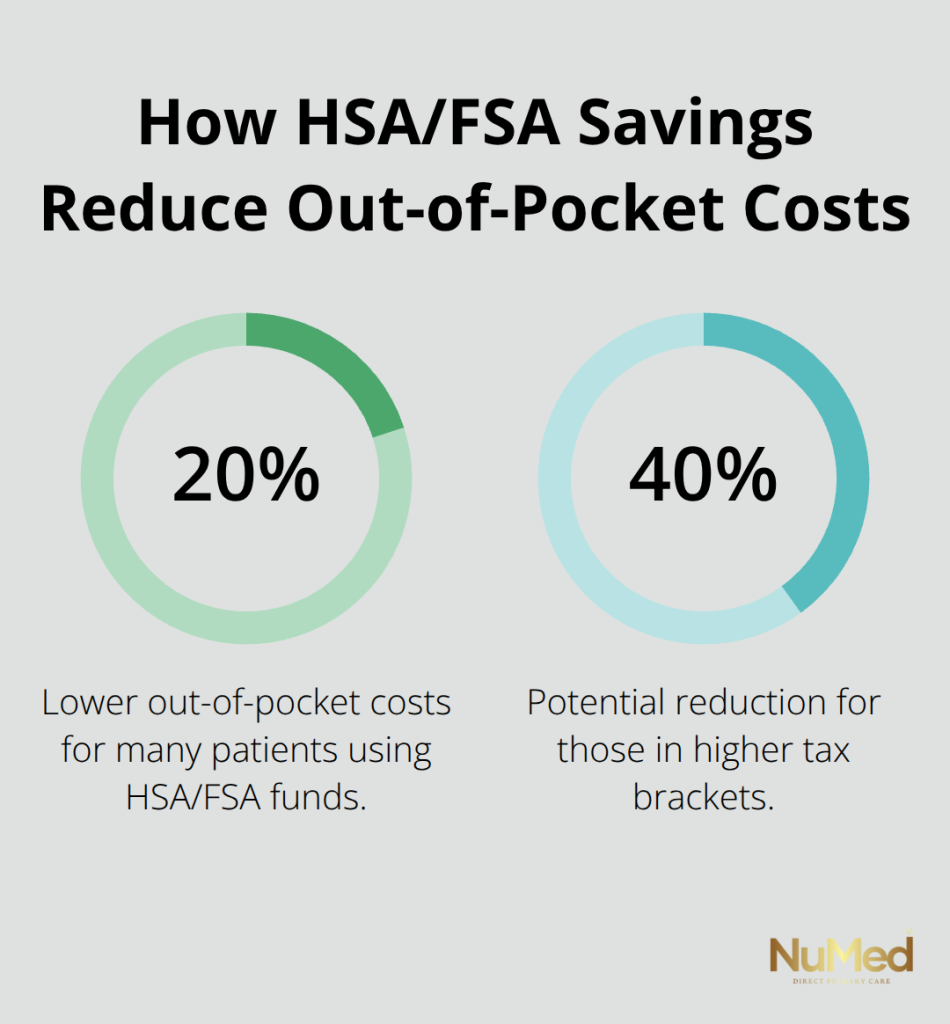
Insurance reimbursement for functional medicine is inconsistent and requires homework before your first visit. Standard labs like CBC, metabolic panels, and lipid panels are covered by most plans, but specialty testing like gut microbiome analysis, SIBO breath tests, DUTCH hormone panels, and genetic testing typically are not. Ask your practitioner’s office to provide a cost estimate before ordering specialty tests and request a superbill for out-of-network submission to your insurance, which sometimes yields partial reimbursement depending on your plan. Health savings accounts and flexible spending accounts cover many functional medicine services if you have access to either, which effectively reduces your out-of-pocket cost by 20 to 40 percent, depending on your tax bracket. The biggest expense surprise comes from lifestyle coaching and extended follow-up visits, which insurance treats as non-covered services.
A nutrition consultation or stress management coaching session might cost 150 to 300 dollars per session, and meaningful behavior change typically requires four to six sessions over three months. Budget for this upfront rather than abandoning the program halfway through.
Alignment Between Practitioner Approach and Your Health Reality
Your functional medicine practitioner’s philosophy about testing and treatment must match your goals and constraints. Some practitioners order extensive genetic testing, micronutrient panels, and advanced imaging as routine, which inflates costs without changing your treatment plan. Ask specifically how they decide which tests to order and what threshold they use before recommending specialty testing. A practitioner who orders testing only when results will change your management approach costs substantially less than one who routinely orders comprehensive panels for every patient. Discuss your budget constraints directly. If specialty testing would strain your finances, a good practitioner adjusts their approach to start with lifestyle modification and standard labs, reserving specialty testing for later if basic changes do not resolve your symptoms. Clarify expectations about treatment timelines. If you expect to feel dramatically better within two weeks, functional medicine will disappoint you. Most patients experience noticeable improvement within 4 to 12 weeks if they implement dietary and sleep changes consistently, but metabolic healing often requires three to six months. Practitioners who promise rapid transformation through supplement stacks without emphasizing lifestyle fundamentals are selling hope, not medicine. Finally, verify that your practitioner coordinates with your conventional doctor rather than positioning themselves as a replacement for conventional care. Functional medicine works best alongside conventional medicine for medication management, imaging when needed, and specialist oversight. A practitioner who dismisses conventional medicine entirely or discourages you from seeing your primary care doctor raises a significant red flag about their judgment and training.
Final Thoughts
Functional medicine is worth it if you have chronic conditions that conventional care has failed to resolve or if you want to prevent disease before it develops. The evidence shows measurable improvements in quality of life, reduced healthcare costs over time, and better outcomes for patients with autoimmune disease, digestive disorders, hormonal imbalance, and persistent fatigue. Success depends on three factors: finding a qualified practitioner who practices evidence-based functional medicine, committing to behavioral changes around nutrition and sleep, and understanding your insurance coverage before starting care.
Your health situation and what you value most determine whether functional medicine aligns with your needs. If you manage stable, well-controlled conditions and feel satisfied with your current care, functional medicine may not be necessary. If you have spent years seeking answers for unexplained symptoms, tried multiple medications without lasting relief, or want to optimize your health proactively, functional medicine offers a different framework that addresses root causes rather than symptoms alone.
Honest self-assessment reveals whether functional medicine fits your situation. Do you have health problems that conventional care has not solved? Are you willing to change your diet, sleep habits, and stress management practices? Can you commit to at least three to six months of consistent implementation before expecting durable results? If you answered yes to these questions, start by finding a qualified practitioner through the Institute for Functional Medicine directory, confirm their credentials and testing philosophy, and have a direct conversation about costs and timelines before your first visit. Visit NuMed DPC to explore how direct primary care combined with functional medicine principles can support your journey toward optimal health.