Menopause affects roughly 1 million women each year in the United States, yet most receive only symptom-focused treatment that masks problems rather than addresses them. At NuMed DPC, we believe menopause care with functional medicine offers a fundamentally different approach-one that identifies root causes and restores balance across your entire body.
Rather than cycling through medications to manage hot flashes or mood swings, functional medicine looks at why these symptoms appear in the first place. This guide shows you how personalized, comprehensive care can transform your menopause experience.
Why Functional Medicine Investigates Root Causes Instead of Just Treating Symptoms
Conventional menopause care typically works like this: a woman reports hot flashes, so she receives hormone replacement therapy or an SSRI. Night sweats appear, so sleep medication follows. Mood changes emerge, and another prescription gets added. The result is a stack of treatments addressing surface-level problems while the underlying imbalances remain untouched. Functional medicine rejects this approach entirely. We start by asking why these symptoms exist in the first place. According to the Institute for Functional Medicine, 50% of adults have at least one chronic condition, and chronic diseases account for 90% of healthcare costs.
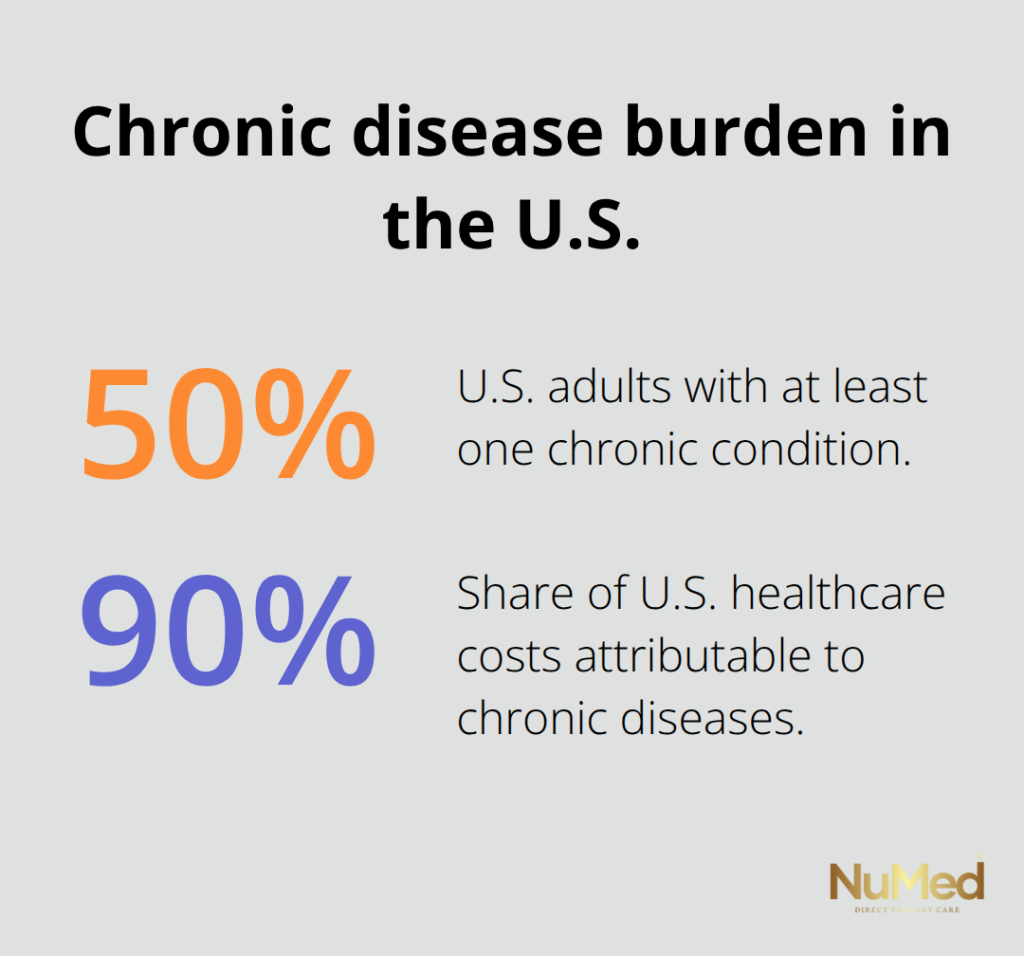
This statistic reveals a healthcare system built on managing disease rather than preventing it. Functional medicine flips that model. When a woman enters a functional medicine practice with menopausal symptoms, practitioners assess her hormone levels through personalized testing, examine her gut microbiome to understand estrogen metabolism, evaluate thyroid and adrenal function, and analyze nutritional deficiencies. They investigate sleep patterns, stress levels, exercise habits, and food sensitivities. They look at environmental toxins and endocrine disruptors in personal care products and home environments. This comprehensive assessment takes time-time that allows for a thorough discussion of your symptoms and medical history rather than rushing through a standard 15-minute visit.
Advanced Testing Reveals Your Actual Physiology
Hormone testing in functional medicine goes far beyond the basic FSH and estrogen panels that conventional doctors order. Practitioners use advanced testing to measure specific hormone metabolites, assess how your body processes estrogen through the gut, and identify whether your symptoms stem from hormone deficiency, poor hormone metabolism, or something else entirely. Thyroid dysfunction affects energy, mood, and metabolism during menopause, yet many women receive reassurance that their thyroid is normal based on a single TSH test. Functional medicine practitioners evaluate free T3, free T4, thyroid antibodies, and reverse T3 to catch patterns that standard testing misses. Gut health testing reveals whether your microbiome can effectively reabsorb estrogen, which directly influences hot flash severity and mood stability. Advanced cardiovascular testing assesses particle size, inflammation markers, and genetic risk rather than relying on basic cholesterol numbers. This targeted data allows practitioners to build treatment plans that address your actual physiology, not a generic menopause template.
Personalized Plans That Match Your Unique Situation
Once practitioners understand your root causes, treatment becomes genuinely personalized. One woman’s hot flashes may stem from poor estrogen metabolism and gut dysbiosis, requiring bioidentical hormone replacement combined with targeted probiotics and dietary changes. Another woman’s hot flashes may result from blood sugar dysregulation and chronic stress, requiring different interventions entirely. Practitioners integrate nutrition, movement, stress management, and hormonal support into a coordinated plan designed specifically for you. This integration matters because menopause involves interconnected systems, not isolated problems. Sleep quality affects cortisol, which affects estrogen metabolism, which affects hot flash frequency. Dietary choices influence gut bacteria, which influence hormone reabsorption. Stress management impacts the hypothalamic-pituitary-adrenal axis, which regulates reproductive hormones. A functional medicine approach recognizes these connections and builds strategies that work synergistically rather than as separate interventions. Understanding how your body’s systems interact with each other sets the stage for the practical tools that actually produce results.
What Results Can You Actually Expect From Functional Medicine Menopause Care
Symptom Relief Happens When Root Causes Shift
Functional medicine delivers measurable shifts in how women experience menopause because it addresses the physiological drivers behind symptoms rather than masking them with medications. When practitioners optimize your estrogen metabolism through gut healing, balance blood sugar to stabilize cortisol, and correct nutritional deficiencies, hot flashes often decrease in frequency and intensity within weeks. Night sweats respond similarly when thyroid function normalizes, and sleep architecture improves through targeted interventions. The North American Menopause Society recognizes that symptom relief happens faster when treatment targets root causes instead of applying generic protocols to every patient.
Women report improved mood, sharper cognition, and sustained energy because functional medicine practitioners address the interconnected hormonal and metabolic systems driving these symptoms, not just prescribe medications for individual complaints. Bioidentical hormone replacement therapy becomes far more effective when combined with corrected gut dysbiosis, optimized nutrient status, and stress management, because your body can actually process and utilize hormones properly. This matters because functional medicine’s integrated approach produces better tolerability and outcomes by fixing underlying imbalances first.
Long-Term Health Protection Extends Beyond Symptom Relief
Menopause increases your risk for osteoporosis, cardiovascular disease, anxiety, and depression, according to the National Institute on Aging, yet conventional care rarely addresses these risks proactively. Functional medicine practitioners prioritize bone density preservation through resistance training, adequate calcium and vitamin D from food sources like leafy greens and fortified foods, and targeted supplementation when testing reveals deficiencies. Cardiovascular protection happens through a Mediterranean-style diet rich in omega-3 fatty acids from fatty fish and flaxseed, which the American Heart Association links to favorable long-term health outcomes.
Mood stability and cognitive function improve when practitioners address inflammation, optimize nutrient absorption, and manage stress through techniques like mindfulness-based stress reduction or cognitive behavioral therapy (both have demonstrated benefits for anxiety and depression during menopause, according to the NIH National Center for Complementary and Integrative Health). This forward-looking approach means you’re not just feeling better now-you’re building the metabolic and hormonal foundation for healthy aging decades ahead.
How Personalized Testing Informs Better Outcomes
Advanced hormone testing reveals whether your symptoms stem from hormone deficiency, poor hormone metabolism, or interconnected system dysfunction. Thyroid evaluation that includes free T3, free T4, thyroid antibodies, and reverse T3 catches patterns that standard TSH testing misses, directly improving treatment accuracy. Gut health testing shows whether your microbiome can effectively reabsorb estrogen, which directly influences hot flash severity and mood stability.
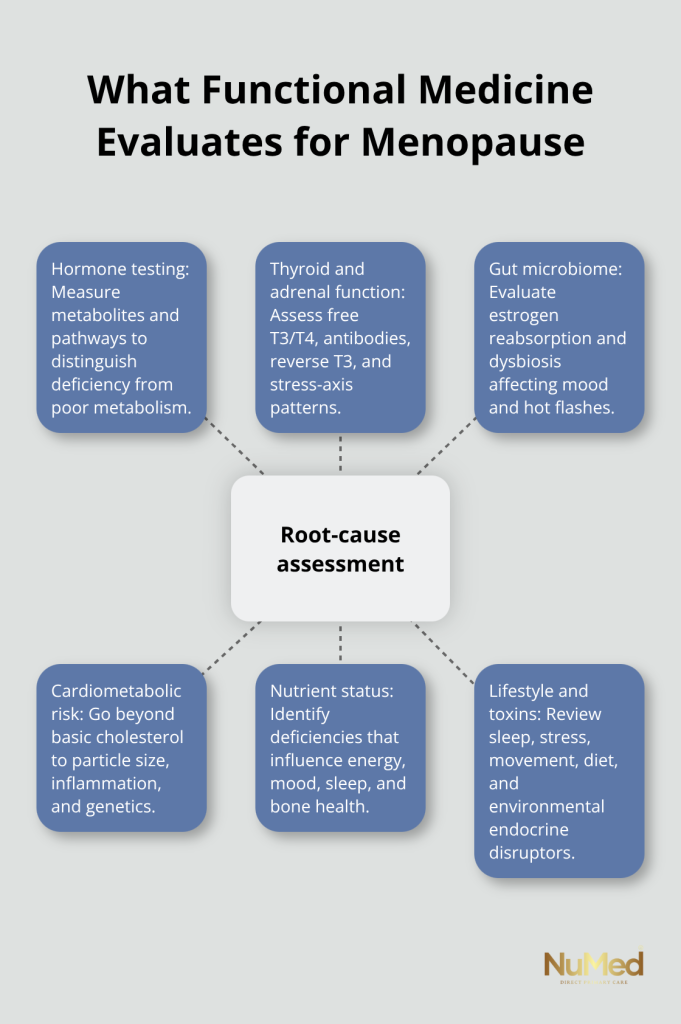
Advanced cardiovascular testing assesses particle size, inflammation markers, and genetic risk rather than relying on basic cholesterol numbers.
This targeted data allows practitioners to build treatment plans that address your actual physiology, not a generic menopause template. One woman’s hot flashes may stem from poor estrogen metabolism and gut dysbiosis, requiring bioidentical hormone replacement combined with targeted probiotics and dietary changes. Another woman’s hot flashes may result from blood sugar dysregulation and chronic stress, requiring different interventions entirely. Practitioners integrate nutrition, movement, stress management, and hormonal support into a coordinated plan designed specifically for you, which sets the stage for understanding how direct primary care models make this comprehensive approach actually accessible.
What Actually Works for Managing Menopause
Dietary Patterns That Reduce Symptoms and Protect Long-Term Health
Mediterranean-style eating patterns produce measurable results during menopause because they address both symptom relief and disease prevention. The American Heart Association links these patterns to favorable long-term cardiovascular outcomes, making them far more than generic healthy eating advice. Fatty fish rich in omega-3 fatty acids, leafy greens loaded with calcium and magnesium, legumes containing phytoestrogens, and olive oil form the foundation of this approach. Phytoestrogens from soy, flaxseed, and legumes offer mild relief from hot flashes for some women, so including soy foods like tofu or soy milk becomes actionable rather than theoretical.
What you eliminate matters equally. Limiting highly processed foods, added sugars, caffeine, and alcohol directly reduces hot flash frequency and improves sleep quality, according to Mayo Clinic research. Magnesium deficiency worsens sleep disruption and anxiety, so prioritizing magnesium-rich foods like pumpkin seeds, almonds, and dark leafy greens addresses root physiology rather than masking symptoms with sleep medication. Calcium and vitamin D from food sources like dairy, fortified cereals, and sensible sun exposure work synergistically to prevent the bone density loss that accelerates postmenopause, according to the NIH Osteoporosis and Related Bone Diseases National Resource Center.
Supplementation becomes targeted rather than random when practitioners test your actual nutrient status first. This testing reveals whether your symptoms stem from a deficiency or from poor absorption caused by gut dysbiosis, allowing treatment to address the real problem rather than guessing. Natural supplements work best when selected based on your individual needs rather than general recommendations.
Movement and Exercise Preserve Bone Density While Stabilizing Mood
Resistance training and weight-bearing activities like walking or hiking directly preserve bone density while improving cardiovascular health, yet many women abandon exercise, thinking hot flashes make it impossible. The reality contradicts this assumption: regular physical activity improves sleep quality, stabilizes mood, and reduces hot flash severity according to the National Institute on Aging. Consistent movement becomes non-negotiable rather than optional when you understand its physiological impact on the systems driving your symptoms.
Exercise produces measurable changes when structured correctly rather than approached haphazardly. Women who maintain resistance training throughout menopause protect their skeletal health while simultaneously improving metabolic function and cardiovascular resilience. The combination of weight-bearing exercise and adequate nutrition (particularly calcium and vitamin D) creates a protective effect against osteoporosis that medication alone cannot replicate.
Stress Management and Sleep Optimization Address Root Drivers
Stress management through mindfulness-based stress reduction, cognitive behavioral therapy, or yoga and tai chi produces measurable benefits for reducing hot flash frequency and severity. These approaches work because they regulate the hypothalamic-pituitary-adrenal axis, which directly influences reproductive hormone balance and cortisol rhythms during menopause.
Sleep optimization happens not through medication but through consistent sleep timing, cool bedroom temperatures around 65 to 68 degrees Fahrenheit, and elimination of blue light exposure one hour before bed. These interventions support the circadian rhythm disruption that drives night sweats and mood instability during menopause.

Your sleep environment and pre-sleep routine directly influence whether your nervous system can downregulate properly, which affects both hot flash severity and next-day mood stability.
Metabolic Timing and Blood Sugar Stability
Time-restricted eating patterns that compress your eating window to eight or ten hours improve metabolic health and hormone metabolism, though this approach requires individualized assessment. Such patterns affect blood sugar stability and cortisol rhythms differently depending on your baseline physiology, so what works for one woman may not suit another. Practitioners evaluate your specific metabolic profile before recommending this strategy, ensuring the intervention supports rather than stresses your system.
Blood sugar dysregulation worsens hot flashes, mood swings, and energy crashes during menopause because unstable glucose triggers cortisol spikes, which suppress progesterone and destabilize estrogen metabolism. Stabilizing blood sugar through balanced meals containing protein, healthy fats, and complex carbohydrates addresses a root cause rather than treating symptoms after they appear. This metabolic foundation supports all other interventions, making it foundational to comprehensive menopause care.
Final Thoughts
Functional medicine transforms menopause from a condition you endure into a physiological transition you actively manage. The difference lies in addressing why your body experiences hot flashes, mood shifts, and sleep disruption rather than simply suppressing these signals with medications. When practitioners investigate your hormone metabolism, gut health, thyroid function, and nutritional status, they uncover the actual drivers behind your symptoms, producing faster relief and lasting protection against the chronic diseases that menopause increases your risk for.
Personalized care delivers measurable outcomes because treatment matches your unique physiology rather than applying generic protocols to every patient. One woman’s night sweats stem from gut dysbiosis affecting estrogen reabsorption, while another’s result from blood sugar dysregulation triggering cortisol spikes-advanced testing reveals these distinctions and allows practitioners to build integrated strategies combining bioidentical hormone replacement, targeted nutrition, movement, and stress management specifically for you. This coordination matters because menopause involves interconnected systems, and optimizing one system without addressing others leaves you partially treated and vulnerable to ongoing symptoms.
The practical tools discussed throughout this guide-Mediterranean-style eating, resistance training, stress management, and sleep optimization-work because they address root physiology rather than masking problems. When you combine these strategies with personalized hormone testing and professional guidance, you produce relief within weeks while building the metabolic foundation for healthy aging. If you’re ready to experience menopause care with functional medicine that prioritizes your actual health rather than insurance constraints, NuMed DPC offers the comprehensive, personalized approach outlined here through our direct primary care model.