Hormones regulate everything from your energy levels to your mood, yet most people never think about them until something feels off. At NuMed DPC, we see patients daily who struggle with fatigue, weight gain, and brain fog-all signs their hormones need attention.
The good news is that natural hormone balance tips don’t require expensive treatments or medications. Small changes to your nutrition, sleep, stress management, and exercise can shift your hormonal health significantly.
What Causes Hormone Imbalance and How It Affects You
The Five Hormones That Control Your Health
Your body produces over 50 hormones daily, with five key players-cortisol, sex hormones, melatonin, insulin, and thyroid hormones-controlling your metabolism, mood, fertility, and blood sugar regulation. When these hormones fall out of sync, the effects ripple through your entire system. Fatigue, unexplained weight changes, mood swings, irregular periods, and brain fog signal that your hormonal system needs attention.

The American Heart Association reports that women should limit added sugar to 24 grams daily to support insulin sensitivity, yet the average woman consumes far more, creating chronic blood sugar spikes that destabilize hormones. Hormone imbalance develops gradually, and many people attribute symptoms to aging, stress, or poor sleep rather than recognizing the underlying hormonal dysfunction.
How Daily Habits Control Your Hormones
Your lifestyle choices are the primary lever controlling your hormonal health, not genetics or age. Sleep deprivation elevates cortisol and stress hormone regulation, which then suppresses thyroid function and promotes fat storage around your midsection. Getting 7 to 9 hours nightly isn’t a luxury-it’s foundational biochemistry. Chronic stress keeps cortisol elevated, which depletes progesterone and sex hormones, triggering mood instability and irregular cycles.
Nutrition and Exercise Shape Hormone Production
Regular aerobic exercise improves insulin sensitivity and blood sugar regulation, with higher-intensity training showing stronger effects, particularly in non-obese individuals. Nutrition shapes hormone production at the cellular level: adequate protein, 25 to 30 grams per meal, provides the amino acids your body needs to manufacture hormones, while healthy fats at roughly 20 percent of daily calories support hormone synthesis. These aren’t minor optimizations; they’re the difference between feeling depleted and feeling vital. Understanding these mechanisms reveals why the next section focuses on specific nutritional strategies that target hormone optimization directly.
What You Eat Directly Controls Your Hormones
Your food choices function as hormone-regulating tools, not just calories. The specific nutrients and timing of meals determine whether your cortisol stays elevated, your insulin spikes dangerously, or your sex hormones stay balanced. Protein intake matters most: try 25 to 30 grams per meal to provide the amino acids your body uses to manufacture hormones like cortisol and progesterone. Without adequate protein, your body cannot produce sufficient quantities of these regulatory molecules. Healthy fats should comprise roughly 20 percent of your daily calories, with omega-3 fatty acids from fatty fish like salmon consumed several times weekly to reduce inflammation that destabilizes hormones.

Cruciferous vegetables, including broccoli, cauliflower, and kale, support liver estrogen metabolism through enzyme activation. For glucoraphanin to be broken down into sulforaphane, an enzyme that’s activated by chewing and chopping these vegetables is required. Fiber-rich foods like oats, lentils, and chia seeds help your body eliminate excess hormones through the estrobolome (the gut bacterial ecosystem that metabolizes estrogen). The National Library of Medicine confirms fiber matters for hormone detoxification, yet the average American consumes only 15 grams daily when 25 to 30 grams is the minimum target. Added sugar directly sabotages hormone balance by triggering insulin spikes that suppress progesterone and accelerate cortisol elevation, which explains why the American Heart Association recommends women limit added sugar to 24 grams daily. Most processed foods contain far more than this threshold, making whole-food eating non-negotiable for hormone stability.
Meal Structure Prevents Blood Sugar Crashes
Meal timing and composition control whether your blood sugar rises gradually or spikes violently. Build every meal and snack around protein, fiber, and healthy fats together-never eat carbohydrates alone. A practical breakfast might be eggs with cheese, spinach, and whole-grain toast rather than oatmeal with fruit. For snacks, pair an apple with peanut butter or choose a corn tortilla with beef, peppers, onions, garlic, beans, and avocado. These combinations stabilize insulin, preventing the metabolic chaos that disrupts sex hormones and thyroid function.
Gut Health Amplifies Nutritional Benefits
Your gut health amplifies these benefits through the estrobolome. Fermented foods like kimchi and yogurt support beneficial bacteria, while prebiotics from garlic and onions feed the microbes that help recycle estrogen. This bacterial ecosystem directly influences your circulating hormone levels, making gut support as important as the nutrients you consume.
Limit Substances That Elevate Hormones Unpredictably
Caffeine and alcohol elevate estrogen and cortisol unpredictably, so limit caffeine to under 200 milligrams daily and alcohol to three drinks per week for women. These substances interfere with the steady hormone regulation that whole-food nutrition provides, undoing your dietary progress.
Reduce Endocrine Disruptors in Your Environment
Endocrine disruptors in plastics, pesticides, and personal care products interfere with hormone receptors at the cellular level. Swap plastic containers for glass or stainless steel, use a water filter, and choose organic produce for high-residue foods like strawberries and spinach. Resources like the Environmental Working Group provide lists of safer personal care products to minimize chemical exposure that undermines your nutritional efforts. These environmental modifications work alongside your dietary choices to create a hormone-supporting ecosystem both on your plate and in your home, setting the stage for the lifestyle modifications that amplify these nutritional gains.
How Movement, Stress Relief, and Sleep Drive Hormonal Stability
Exercise Rewires Your Hormonal Signaling
Exercise transforms your hormonal baseline far beyond calorie expenditure. Higher-intensity training produces stronger effects on insulin sensitivity and hormone regulation than moderate activity, particularly in non-obese individuals. You don’t need gym equipment or complicated routines: regular aerobic exercise, strength training, and high-intensity interval training all improve your hormonal foundation, but consistency matters far more than intensity spikes. Research shows that daily movement outperforms sporadic workouts, meaning a 20-minute walk most days surpasses an occasional intense session. Try 150 minutes of moderate aerobic activity weekly, combined with strength training twice weekly to preserve muscle mass that supports metabolic hormones. Overtraining suppresses hormones, so avoid the trap of thinking more exercise always means better results-your body needs adequate recovery and nutrition to produce the hormones that make exercise beneficial in the first place.
Stress Management Lowers Cortisol Directly
Stress management directly lowers cortisol, the hormone that sabotages everything else when chronically elevated. Mindfulness-based stress reduction and cognitive-behavioral therapy both improve hormone-related symptoms and quality of life, with research showing measurable improvements in sleep quality and vasomotor symptoms during hormonal transitions. Implement a specific stress-relief practice rather than vague goals: the 4-7-8 breathing technique (inhale for 4 counts, hold for 7, exhale for 8) activates your parasympathetic nervous system and reduces cortisol within minutes. Social connection lowers cortisol more effectively than isolation, so prioritize time with people who support your wellbeing.
Sleep Quality Determines Whether Other Efforts Succeed
Sleep quality determines whether your other efforts succeed or fail. Research shows that sleep disruption during hormonal transitions affects estrogen regulation and destabilizes every other hormone. Try 7 to 9 hours nightly with a consistent sleep schedule, going to bed and waking at the same times, even on weekends. Your bedtime routine matters: dim lights at least one hour before sleep, eliminate screens 30 to 60 minutes beforehand, and keep your bedroom cool around 65 to 68 degrees Fahrenheit. Foods high in magnesium and tryptophan support melatonin production-include nuts, dairy, leafy greens, salmon, whole grains, and tart cherries in your evening meals. These three pillars (regular exercise, targeted stress relief, and protected sleep) amplify the nutritional foundation you’ve already established, creating the conditions where your hormones stabilize naturally.
Final Thoughts
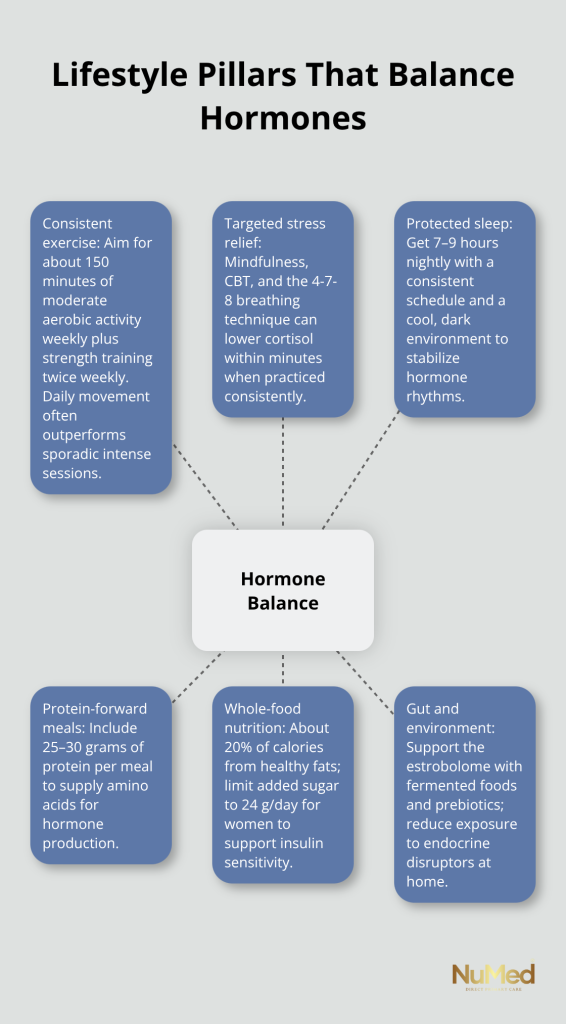
Hormonal balance emerges from consistent application of natural hormone balance tips across nutrition, movement, stress management, and sleep rather than from a single intervention or supplement. Protein at every meal, whole foods over processed options, regular exercise, stress relief practices, and protected sleep create the biochemical conditions where your hormones stabilize naturally, with most people seeing measurable improvements in energy, mood, and weight within 4 to 8 weeks. These strategies work because they address the root causes of hormonal dysfunction rather than masking symptoms.
Some hormonal imbalances require professional evaluation, particularly if you experience unexplained weight changes, heart palpitations, severe mood disturbances, or infertility despite months of lifestyle modifications. Advanced hormone testing through blood and saliva analysis maps your specific hormonal patterns and reveals whether your cortisol, estrogen, testosterone, or thyroid hormones need targeted intervention. Medical testing can identify underlying thyroid dysfunction, insulin resistance, or other conditions that need clinical support.
Start with foundational changes-prioritize sleep, build meals around protein and fiber, and move your body consistently-then track how you feel over the next month. If progress stalls or symptoms persist, NuMed DPC combines functional medicine with personalized health coaching to address hormonal health comprehensively and accelerate your results. Hormonal wellness is achievable, and the path forward begins with the choices you make today.